
How can journalism be useful? Working with grassroots groups to investigate health exclusion
How can we be useful? It’s a simple question, but how often do we ask it as journalists? In the years I spent working for a union, I collaborated with reporters on hundreds of stories across print and broadcast media, but I can count on one hand the number of times a journalist asked me that question.
But that was the question we asked repeatedly when, together with grassroots migrant support organisations, we designed the investigation that uncovered how an huge number of undocumented migrants were being refused registration with GP surgeries. By asking this early on, and building a genuine collaborative relationship with groups representing the people directly affected by the issue, we ensured that months later our reporting was able to make a meaningful impact on the ground.
We knew in the spring that despite glowing headlines about the UK’s vaccine programme, something did not add up. For years, the government’s so-called “hostile environment” policy had made the National Health Service an increasingly unwelcoming institution for the hundreds of thousands of undocumented migrants living in the UK. Although government ministers gave assurances that everyone had the right to receive the vaccine, we suspected it would not be enough to overturn the culture of exclusion that had been built over last past decade.
Months before, Haringey Welcome, a migrant support organisation, had done a secret shopper survey of some of the GP surgeries in the north London borough. They found that despite the fact undocumented migrants had the right to register with a GP, many surgeries would turn them away, either because they didn’t have ID, proof of address or proof of immigration status.
We spoke to Haringey Welcome and other groups that were advocating for more equitable access to the vaccine, including Migrants Organise, MedAct and Doctors of the World, to see if migrants were still facing these barriers. With GP surgeries such as key part of the roll-out, were people were missing out on being vaccinated?
These conversations shaped our reporting. We adapted the survey methodology that had been developed by Haringey Welcome, added questions about vaccine access, picked 10 cities where we would roll out the survey across over 200 surgeries, and worked on a timeline for the investigation that would ensure that the results made an impact. At every step of the way, we spoke to these organisations to make sure our approach reflected their experiences on the ground and that our reporting would build an accurate dataset.
Collaborating with organisations that are fighting to redress social inequalities is part of Bureau Local’s ethos. While we might not always get it right and it might not work for every story, in this instance it was clear from the beginning that this was the only way to make a strong, enduring impact.
We did not try to reinvent the wheel: Haringey Welcome and other groups had already designed the basis for this style of research. Nor was it a matter of taking up space occupied by advocacy organisations. Instead, it was about starting an honest conversation about how we could build on their methods in order to produce a body of evidence that would, in turn, help their campaign for a more equitable health system.
As one NHS England inclusion lead told us after we published the investigation, our findings give “a robust account of the reality that's hidden from people unless they’ve experienced it”.
Being transparent about our intentions, methodology and timing were key to building trust and led to a closer working relationship, which benefited everyone. We were kept abreast of developments on the ground, such as the announcement of new pop-up vaccination centres or the creation (and later removal) of a government portal listing local vaccination centres. Meanwhile, grassroots organisations were able to build their comms and campaign strategies around our publication timeline and, once the story had gone out, to use our findings to drive change.
For example, Doctors of the World built a “Write to your MP” tool, which they released in conjunction with the publication of our investigation. To date, more than 1,000 emails have been sent to 425 MPs, raising concerns over the way undocumented migrants are denied access to GPs.
Activists and community groups also used our data to apply pressure and educate their local surgeries and health bodies. A local branch of the Patients Not Passports campaign sent a letter to all surgeries in Manchester with our findings, while individuals in Stockport, Suffolk and London wrote to representatives of their local clinical commissioning groups asking them to ensure that surgeries were registering undocumented people.
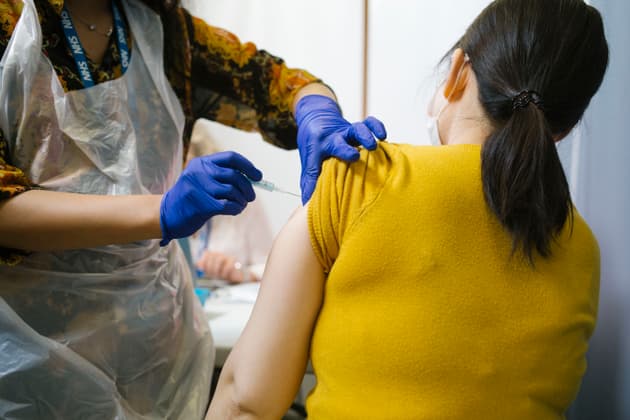 Many migrant communities face problems accessing NHS services
Photo by Alex Sturrock
Many migrant communities face problems accessing NHS services
Photo by Alex Sturrock
On the ground, the impact has gone even further. For the first time, the British Medical Association – the professional body for medical professionals – officially endorsed Doctors of the World's Safe Surgeries programme, which ensures that local practices follow NHS registration policies. Doctors of the World says that since the publication of the Bureau’s investigation, 50 more surgeries across the UK have joined the programme, and engagement on this issue has improved with local health bodies such as clinical commissioning groups and primary care networks. We even heard from people who sought help in getting vaccinated after seeing the investigation.
But our work didn’t end once the article was published. Once the dust settled, we made an effort to brief decision makers – from NHS England representatives to MPs — on our findings.
There is still a long way to go. Our follow-up investigation found that the Care Quality Commission, the healthcare regulator, was rating the majority of the surgeries refusing to “good” and refusing to recognise that there was a problem.
But the investigation has helped move the dial, and provided the biggest data-set so far on the way undocumented migrants are excluded from primary care. We would never have made such an impact if we hadn’t collaborated from the start with the grassroots groups that for years had been doing the vital work to address these inequities, and if we hadn’t asked that simple question: how can we be useful?




