Superbugs more common in people who have travelled to Asia or Middle East
People who have travelled to areas of the world with high rates of antibiotic resistant bacteria such as South Asia and the Middle East are more likely to carry superbugs, a new study has found.
Even having a housemate who has travelled to these areas increases the chance of carrying resistant gut bacteria called ESBL producing Enterobacteriaceae, the research showed.
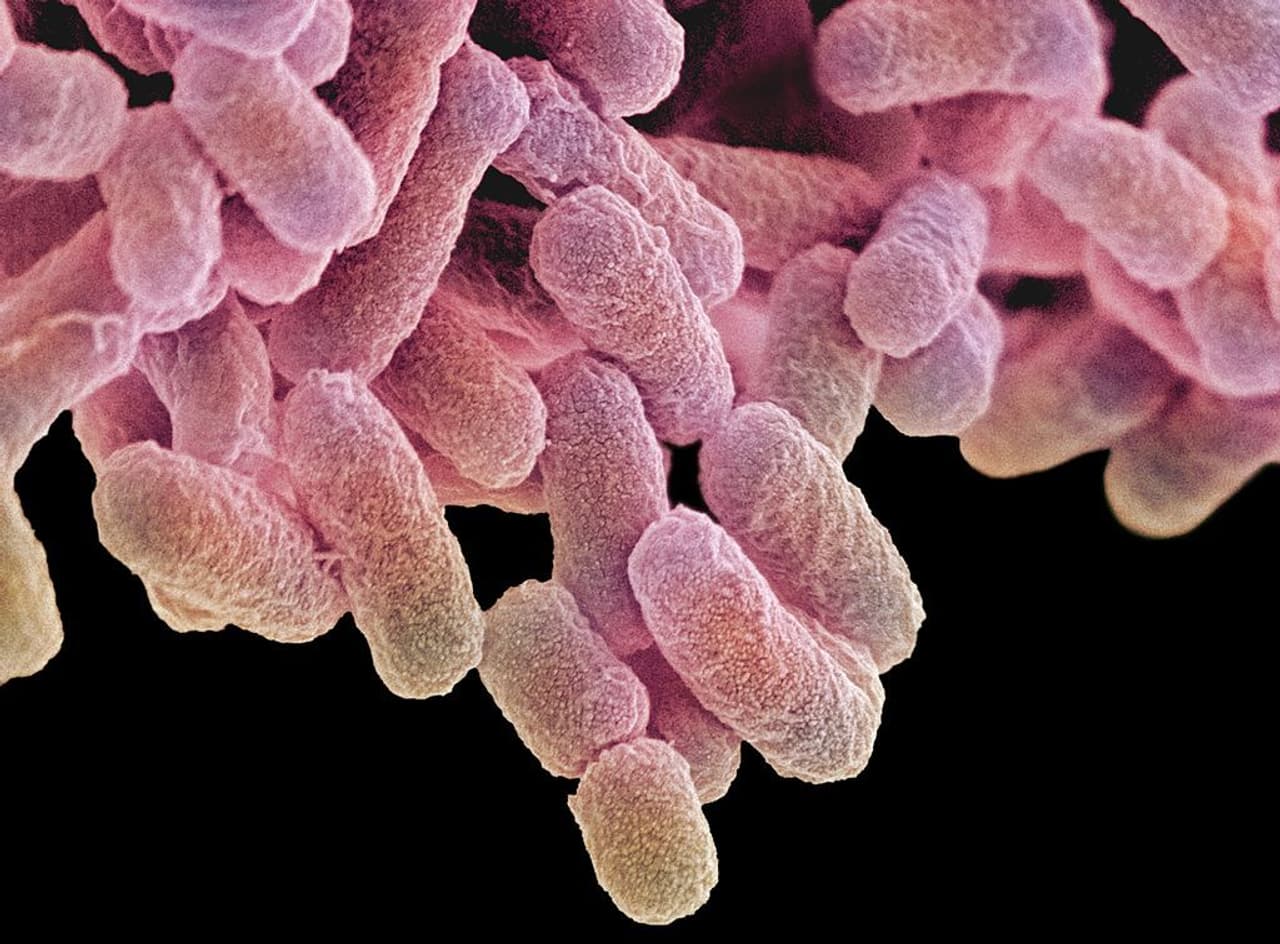
Enterobacteriaceae are bacteria such as E.coli and Klebsiella which everyone carries in their bowel harmlessly and with no symptoms. Yet occasionally they can get into the wrong part of the body and cause wounds, urinary tract, lung and bloodstream infections which can be deadly.
They are part of the gram negative family of bacteria known to be becoming much more resistant to antibiotics. If the bacteria have ESBL genes they are resistant to two classes of antibiotics – penicillins and cephalosporins – normally used to treat these infections. This forces doctors to turn to other drugs. Once a person becomes colonised with these superbugs they remain in their gut for six months to a year.
“The findings show the problem of antibiotic resistance is global and that bugs bred in one country quickly spread to another due to global travel”, said Professor Peter Hawkey, a microbiologist at the University of Birmingham who carried out the research.
It is overuse and misuse of antibiotics that has led to bacteria with ESBL genes forming, and they are just one type of superbug. Across many parts of Asia and other developing countries it is possible to buy antibiotics over the counter with no prescription or diagnosis, for use on humans and on livestock. This has led to unchecked and inappropriate consumption, which fuels resistance to the drugs.
Issues with hygiene, water and sanitation in many low and middle income countries exacerbates the problem as it means high numbers of people suffer infectious diseases and carry resistant bacteria in their guts.
“We can’t think that antibiotic resistance is someone else’s problem; it isn’t.” Professor Hawkey said. “Poor sanitation and antibiotic control in one country affects another. We’re all interconnected, we’re all travelling more. The people that are more likely to travel to parts of the world where these bacteria are common are the ones more likely to be carrying them.
“The results show the perfect storm that is gram negative antibiotic resistance. It’s a quiet storm, it’s not a dramatic outbreak, but it could have dramatic effects .”
Make change possible
Investigative journalism is vital for democracy. Help us to expose injustice and spark change
Click here to support usCurrently around 5,000 people are thought to die of resistant infections every year in the UK, though experts say the real figure is likely to be much higher. A government-commissioned review found 700,000 people are dying every year worldwide, with this figure set to rise to 10m by 2050 if no action is taken.
Currently doctors adhere to specific guidelines when they suspect a patient has a resistant infection, such as changing their course of antibiotics or isolating them in a single room so they cannot spread the bacteria to other patients.
“Doctors should take into account this study’s findings and consider a patient’s travel history if they come into hospital with an infection suspected to be from ESBL bacteria”, Prof Hawkey said.
The study was led by Public Health England and the University of Birmingham and published in the Journal of Antimicrobial Chemotherapy. The researchers signed up 2,430 people from GP practices in four different areas of the country and analysed samples of their faeces in the laboratory for the superbugs.
They found 7.3% of people across all areas carried these superbugs, but the prevalence varied greatly across the four parts of the country.
Shropshire, which has a mainly white British population, had a prevalence of 4.9% while the Heart of Birmingham , with a predominantly Asian population, had a prevalence of 16%.
When they broke it down into specific groups of people those with the highest prevalence were those who had travelled to South Asia – India, Pakistan, Bangladesh, Sri Lanka, Nepal – (38.5%) or those born in South Asia (25%).
Living with someone who had visited a high risk country significantly raised the chance of carrying the superbugs. People with a housemate who had travelled to the Indian subcontinent in the last year had a prevalence of 22.7%, while those living with someone who had visited the Middle East had a prevalence of 16.9%.
Doctors were more likely to carry the superbugs than the general population. Age or sex made no difference to the risk of being colonised.
The research echoes other European studies which found travellers to countries outside Europe have a 10-fold higher prevalence of ESBL bacteria than the local population.
A spokesperson for Public Health England said “the results of this study will be used to inform infection management and antibiotic guidance.”