
Womb loss in Malawi - an unfolding tragedy
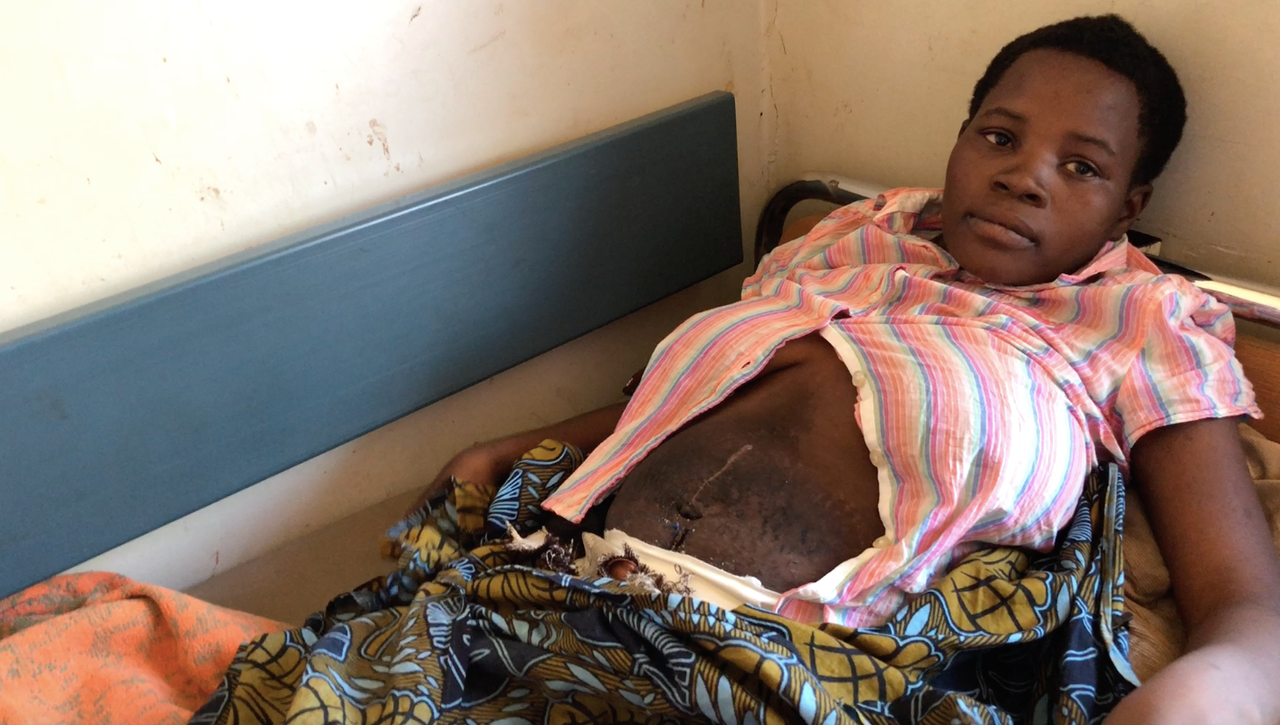
In a dark room in a hospital in Thyolo, a town in the south of Malawi nestled among tea plantations, Ngellina Chikopa was lying on a bed. The 18-year-old unwrapped her chitenje, the sarong worn by Malawian women, to reveal a long wound oozing with pus. The cut stretched from her lower abdomen through her belly button and up past her stomach.
Ngellina gave birth by Caesarean section in April 2018, but the baby died of asphyxia, where the infant becomes stuck and suffers brain damage from lack of oxygen. She should then have had time to grieve; instead, her wound became infected. She was given intravenous antibiotics but the infection raged on and the wound started to release foul-smelling pus. It spread to her uterus. Doctors gave antibiotics but they didn’t work. Doctors at Thyolo hospital were forced to perform a hysterectomy, an operation to remove her womb. This meant she could never bear children in the future.
Later, she suffered another infection and was transferred to Queen Elizabeth Central hospital, a major referral hospital in the city of Blantyre, where she had another two operations to clear the pus and close the wound. She was discharged, but then returned to Thyolo hospital because her stomach was not healing properly. The Bureau visited the hospital during our recent investigation into antibiotic resistance in Malawi. Ngellina was sharing a room with a young woman called Margaret, who had also lost her baby to asphyxia.
Ngellina told us that she feared being ostracised, now that she is no longer able to have children. In Malawi, there is a stigma attached to both being unmarried and childless. “I know that I will never ever have children in my lifetime, I have accepted it with a lot of pain as there is nothing I can do about my situation,” she said. “Some relations are aware of my situation and I know the social discrimination that I will be facing out there.” She hopes to go back to school when she recovers or seek employment.
While rare in the UK, scores of women in Malawi face having their wombs taken out due to infection, according to figures supplied to the Bureau. Dr Martha Makwero, the acting head of the maternity department at Queen Elizabeth Central Hospital said that 36 women had undergone hysterectomies, due to infection, between March and May in 2018 alone.
At Zomba Central Hospital around five people a month had their wombs removed, said Dr Maguy Kabeya, head of the maternity department, who carried out a three month observation this year. He stressed they were all referred from district hospitals and health centres, where infection prevention is poorer. Some of the women died. The Bureau asked other major hospitals in Malawi for figures, but they did not provide them.
Dr Pat O’Brien, a consultant obstetrician at University College London Hospitals (UCLH), said those numbers were “terrible”, adding that having a hysterectomy due to infection was “almost unheard of” in the UK. “I’ve been a consultant at UCLH in London for 19 years and I think I’ve seen that twice in my entire time,” he said.
 Unsanitised equipment pictured in a Malawi hospital
Madlen Davies/the Bureau
Unsanitised equipment pictured in a Malawi hospital
Madlen Davies/the Bureau
Doctors may resort to hysterectomies in Malawi to remove the source of an infection. This is for a variety of factors that all heighten the need for this drastic step. Women are more likely to have suppressed immune systems, due to both malnourishment or diseases like HIV, meaning they are less able to fight off infections a healthy body might easily quash. Some 12.8% of Malawian women are HIV-positive, compared to 8.2% of men, according to a Ministry of Health Impact assessment between 2015 - 2016. Women's diets can be relatively poor and low in both calories and nutrition, often consisting of a restricted amount of fruit or vegetables and carbohydrates.
Additionally, infection control, especially in rural health centres and district hospitals, is poor. More than half of healthcare facilities lack good water and sanitation. This makes it difficult to clean both the hospital itself and equipment used during childbirth.
Electricity blackouts mean equipment used in labour may not be sterilised properly. Hospitals frequently run out of essential supplies like chlorine, soap and antiseptic gloves. Women are asked to bring certain items to the hospital for the birth: a plastic sheet called a macintosh, a razor-blade to cut the cord and a plastic tub to bathe the baby. These aren’t sterile, so they also add to the risk of the mother contracting an infection.
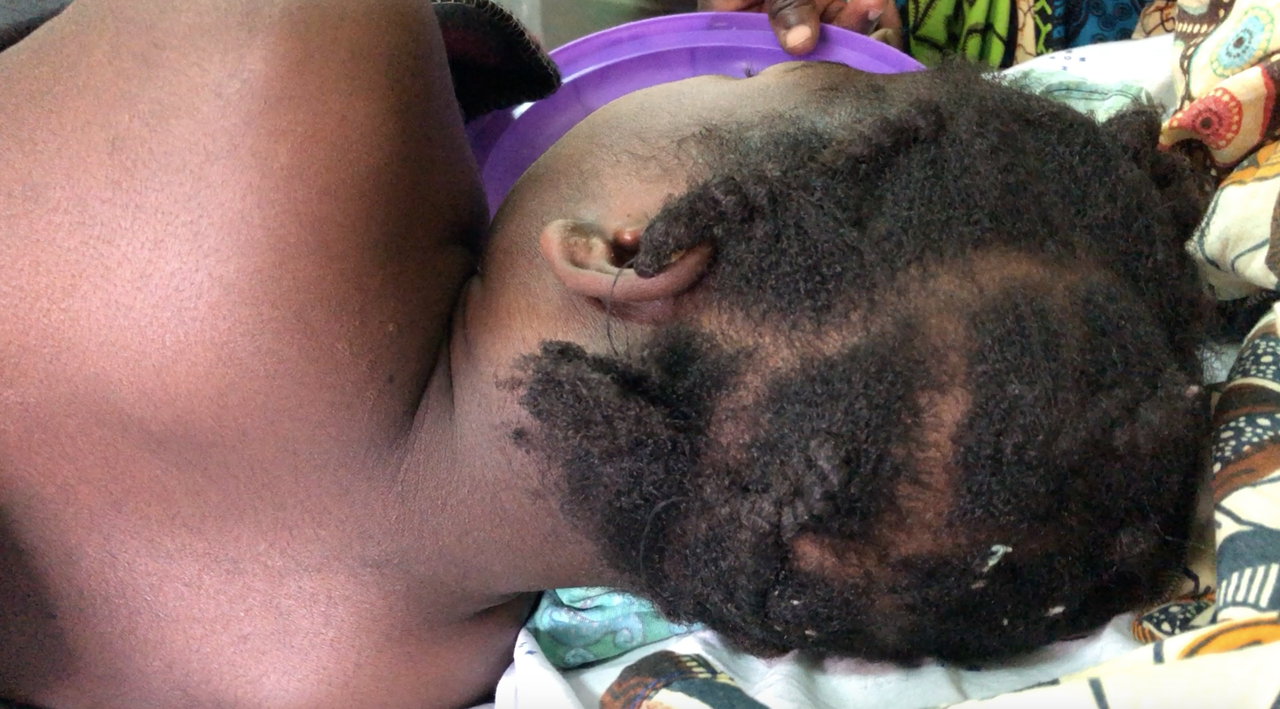
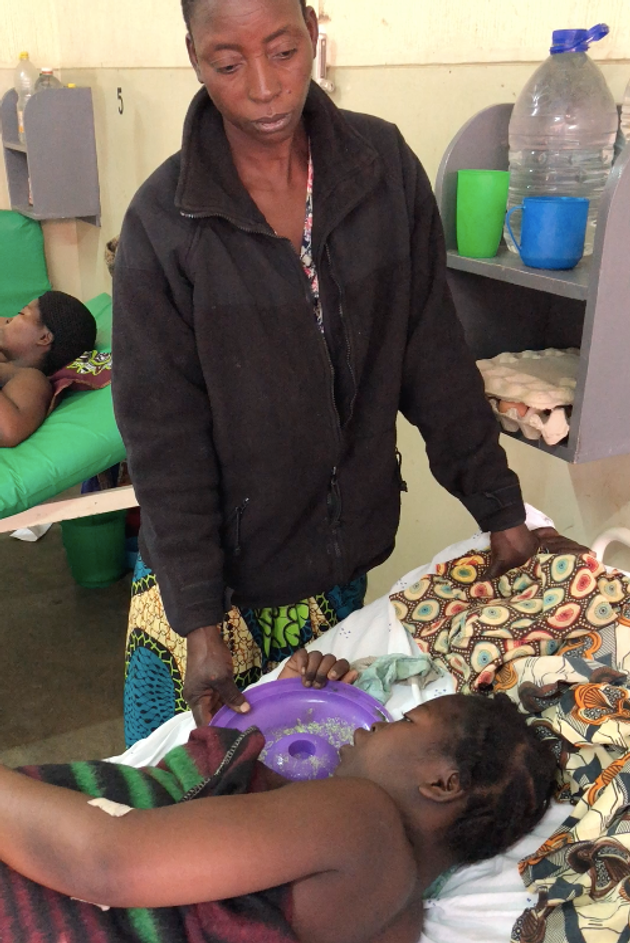 Florence Matandika, pictured with her mother, Judith, in hospital in Blantyre
Madlen Davies/the Bureau
Florence Matandika, pictured with her mother, Judith, in hospital in Blantyre
Madlen Davies/the Bureau
We met Florence Matandika, aged 18, lying in a bed in Queen Elizabeth hospital maternity ward in Blantyre. She was crying out in pain. Her mother Judith, was next to her, holding the lid of a plastic tub onto which Florence occasionally vomited.
Florence was very sick. After a prolonged labour on May 10 she gave birth to a stillborn baby by C-section. The wound from the infection became infected and her stomach started to swell. She was in a lot of pain. The infection then spread to her uterus and doctors were forced to perform an operation to remove it. She was given two types of antibiotics but the infection persisted.
“I have given up on the husband,” said Judith Matandika, Florence’s mother. She added: “I know he will marry another woman because my daughter cannot have children anymore. I’m in pain but I will accept God’s will.”
In Western hospitals every woman is given a dose of antibiotics before a C-section operation to prevent infection. This is not always done in Malawi. In the UK, a blood culture test would also be carried out if the woman did succumb to an infection. A sample of her blood, or a swab from her wound, would be sent to a lab, where technicians would identify which bacteria is causing the infection and which antibiotics could work against it.
But blood culture facilities are expensive; they require sophisticated laboratory equipment and trained staff. Most hospitals in Malawi don’t have access to them. Even Zomba, a referral hospital, sends samples to the lab at Queen Elizabeth hospital in Blantyre if a blood culture needs to be done.
Queen Elizabeth hospital has blood culture facilities as they are provided by the Malawi Liverpool Wellcome Centre, the research institution next door. But they are rationed to adult and paediatric patients. Cultures are rarely sent for women on the maternity ward. There is also a limited number of antibiotics available in most hospitals. Usually only penicillin, gentamicin and ceftriaxone are available to give to pregnant women with infections.
The hospital is now facing a new problem: rising antibiotic resistance. A study by the Malawi Liverpool Wellcome Centre showed that while the number of bloodstream infections fell between 1998 and 2016, the proportion resistant to antibiotics increased sharply.
In Klebsiella, an infection commonly causing bloodstream infections, resistance to the two major classes of antibiotics available in the hospital (penicillins and cephalosporins) rose from just 12% to 2003 to 90% in 2016. In E.coli, a leading cause of sepsis, resistance rose from under 1% to 30% in the same time period.
The data that is available is for adults and paediatric patients, while there is none on the resistance patterns of infections in mothers.
 Images of the Chikopa family, pictured at home
Madlen Davies/the Bureau
Images of the Chikopa family, pictured at home
Madlen Davies/the Bureau

Dr Makwero, the acting head of the maternity department, believes resistance is hampering treatment of women with infections. There are many women for which the antibiotic, ceftriaxone, is not working, Dr Makwero said. “The bugs that we are seeing are resistant to ceftriaxone,” she said. “It really affects our management. We tend to clear the infection through surgery but it is not always working,” she said. She fears for the future as resistance rises. “It would be catastrophic if we could not use ceftriaxone any more,” she said.
For these patients, she has to seek permission to use meropenem, an expensive antibiotic which the hospital doesn’t always have in stock. The head of the department has to sign forms and the pharmacist has to be convinced it is needed. There are concerns using it more frequently would lead to resistance emerging. Rising resistance to meropenem would be disastrous, medics told the Bureau, as it would leave doctors with even fewer options for treatment.
Dr O’Brien accepts that hysterectomies are carried out to save women’s lives. Yet he believes this is a false economy as the operations are far more expensive than a blood culture would be, and much more traumatic. “If it’s truly the case that doing a hysterectomy is the only way to save someone’s life then clearly that’s a better option regardless of all of this. But clearly getting the right antibiotics and blood cultures would be a better way of dealing with this,” he said.
Ngellina’s father Bester lives with her 10-year-old sister Ivy in a straw-roofed house in a nearby village. When we visited, a clothes line ran through their tidy house. Half the dirt floor was covered by pots and pans, a cooking stove, and bags of maize.
Bester, a second-hand clothes salesman talked in an anguished voice about his older daughter’s situation. He had no idea she had a boyfriend, and by the time he was told, Ngellina was pregnant. “Now that the boyfriend is aware of Ngellina’s fate, he seems to have lost interest in her. He has completely disappeared,” he said. He accepted that she had a right to a sex life, but pointed out that she should have had access to contraceptives, avoiding an unexpected pregnancy.
It was difficult for him to see his daughter in pain. Her hospital stay also affected the family's finances. He had to pay for transport, food, and wound dressing cream they had run out of at Queen Elizabeth hospital.
Now, understandably, given the stigma around womb removal, he fears for his daughter’s prospects. “I’m concerned that she lost her baby and she had her uterus removed,” he said. “In our culture, this means a girl has no future at all as no man would be interested to marry her. By removing her uterus, they have taken away the entire future clan from us.”
Translation and fixing support from Josephine Chinele. All pictures in the article photographed by Madlen Davies/the Bureau



