"Another Daesh": Superbugs plague Afghan hospitals
As the conflict in Afghanistan and Iraq evolved, military doctors who were already grappling to treat soldiers maimed by roadside bombs began facing another challenge. Patients were developing multi-drug-resistant infections in their wounds, meaning they couldn’t be treated with usual antibiotics.
Colonel Clinton Murray, 48, an infectious diseases doctor, was deployed to the region four times between 2003 and 2015, working in military hospitals and clinics across the country, and also ran the infectious diseases department at Brooke Army Medical Center in Texas, one of two US hospitals which received soldiers with injuries so bad they had to be evacuated back to America.
He said drug resistant, or ‘superbug’ infections, meant some soldiers had problems for years after their initial life-altering injury. When common antibiotics failed, higher doses of antibiotics, new drug combinations or alternative drugs with severe side effects were tried, but many suffered repeat and prolonged infections. Some had to undergo extra surgeries or amputations because the bacteria couldn’t be stopped and had spread.
The US army soon realised drug resistance was a serious problem and from 2009 onwards introduced programmes in military hospitals to reduce antibiotic resistance. Yet superbugs were an even bigger problem in civilian hospitals without the resources to deal with them, and where civilians could not be evacuated abroad.
Doctors, WHO representatives and NGO workers warn patients in Afghanistan are still dying of drug resistant infections, in a public health crisis that is going undetected, adding strain to a health system vulnerable after decades of conflict.
Afghan citizens are already dying because of the war, but drug resistance will mean even more deaths, said Dr Nasimullah Bawar, head of health programme at BRAC Afghanistan, an NGO providing drugs and maternity, child health, immunisation, nutrition, mental health and malaria and TB control services in four provinces.
He compares superbugs to another scourge, Islamic State or Daesh, because it will disrupt the country and kill high numbers of Afghan citizens: "This is going to be another Daesh, I can say."
US Army intervenes
The military had been struggling with resistant infections since the start of the war but it wasn’t until years later that military physicians identified the scope of the problem.
Infections from a resistant form of one type of bacteria, Acinetobacter baumannii, became so common in Iraq and then Afghanistan the soldiers gave it a nickname: ‘Iraqibacter’. The bug had usually been a problem in older or very sick patients who had spent months in hospital, but doctors were now seeing it in young, fit, soldiers.
At the peak of the problem, between 2004 and 2006, the budget for one class of last resort antibiotics - carbapenems – used for the severe and multi-drug-resistant infections commonly seen in blast wounds, went up by more than 400%.
The use of another drug, colistin, called the ‘last hope’ drug as it is used to save the lives of critically ill patients with multi-drug-resistant infections, became so common the army had to restrict it.
Targeted control programs introduced in military hospitals in 2009, including guidelines on antibiotic use, better surveillance of drug resistance, improved record keeping and better infection control, led to a reduction in cases within six years.
These improvements, combined with the ability to evacuate soldiers back to the US, meant although some died, many survived. “I have folks I’ve been following for 10 to 15 years,” said Murray. “First couple of years we wrestled with infection. Then for the next 11 they’ve done great. You know, they live functional lives.”
He recalls one patient who lost both his legs after being hit by a roadside bomb in Iraq. Three weeks after the blast, back in the US, infections developed in his stumps. Doctors swabbed the wounds and found a plethora of dangerous organisms, including three different types of multi-drug-resistant bacteria: Acinetobacter baumannii, Pseudomonas aeruginosa, Klebsiella pneumoniae as well as Staphylococcus aureus. To stem these infections they had to give him antibiotics which caused kidney failure, though luckily his organs recovered after the drug therapy was stopped a few days later.
The patient went on to suffer more superbug infections. On one occasion the antibiotics given poisoned his bone marrow, which affects the body’s immunity and clotting. He was given a different antibiotic which cleared the infection in that stump, and fortunately the poisoning did not turn out to be permanent. However he developed a superbug infection in his other stump. Doctors suggested more surgery to cut away the infected part of his leg, but he opted to take antibiotics long term to quash the infection instead.
Now, 12 years after being hit, he still has to take antibiotics to keep the infection at bay, but he lives a normal life with prosthetic legs. "His kids and my kids knew each other and now they’re in college and doing great," Murray said.
The same standards of care were not provided to civilians. Superbugs made the civilian population in war zones an object of fear, said Dr Christian Haggenmiller, a former senior NATO medical officer in Afghanistan. Military medical facilities sometimes rejected civilian patients because of fear that they carried resistant bacteria which could infect the intensive care unit (ICU) for military personnel. As a result, they were often treated separately, in isolation tents away from the main medical facilities.
“It’s your worst nightmare, having a drug resistant strain in your health facility that you can’t control. It’s like a new disease,” he said.
Not so lucky civilians
The gains made in military hospitals were not seen in public facilities, which are still struggling with drug resistant infections. The health system in Afghanistan has been fragmented by decades of war, and civilian hospitals are understaffed, underfunded and overburdened.
Despite improvements in recent years, it still has one of the worst healthcare systems globally. One woman dies every two hours from pregnancy-related causes, according to conservative estimates, and one in 25 newborn babies dies - the third highest neonatal death rate in the world.
Life expectancy at birth is 64, compared to 79 in the US and a global average of 72. There is a shortage of doctors, especially in rural areas, and infection control is poor.
Drug resistance has already become one of the world’s greatest public health crises, estimated to cause 700,000 deaths worldwide and expected to kill 10 million by 2050 if no action is taken.
Fuelling the superbug problem in Afghanistan is the unregulated sale of antibiotics in human medicine and in agriculture. Drugs are advertised on television and available to buy over the counter from pharmacies without a prescription or diagnosis from a doctor.
“They give them out like sweets,” said Dr Doris Burtscher, a medical anthropologist at Doctors Without Borders. Burtscher compiled a report in 2015 about attitudes to antibiotics at a public hospital in Kabul and found the drugs were taken for anything from bruised knees to nosebleeds and body pain, as well as by women after menstruating.
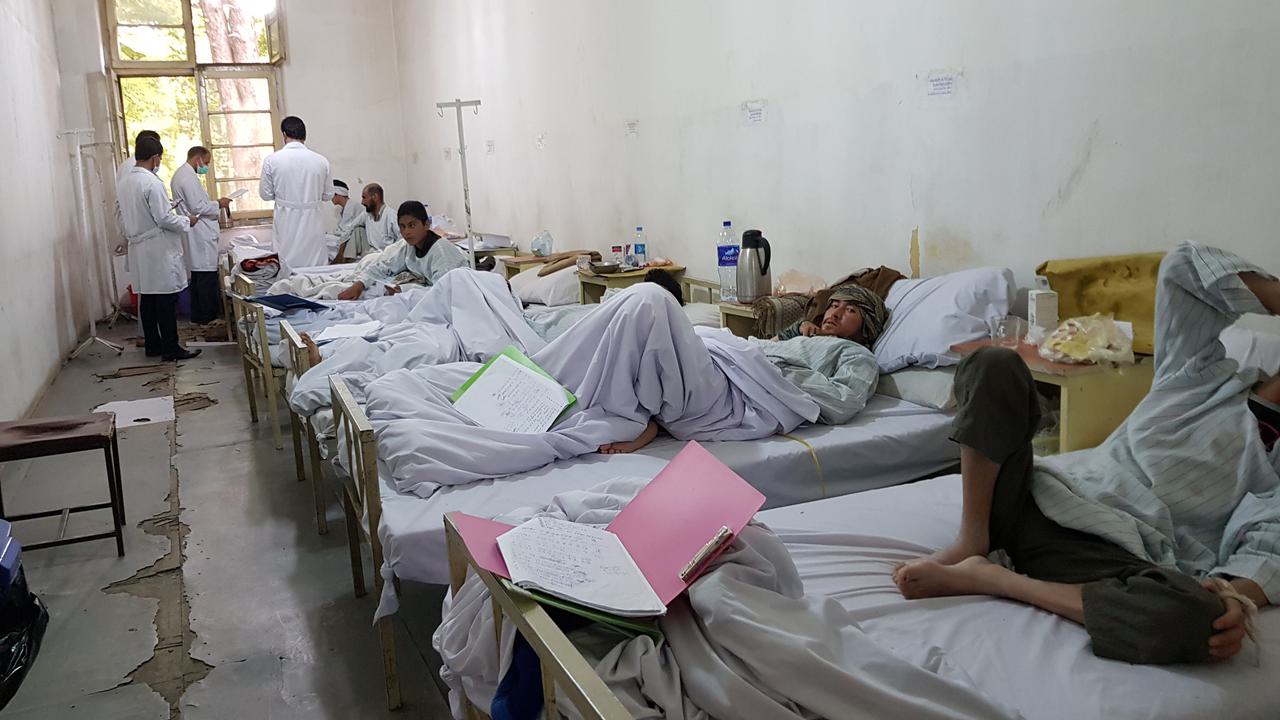
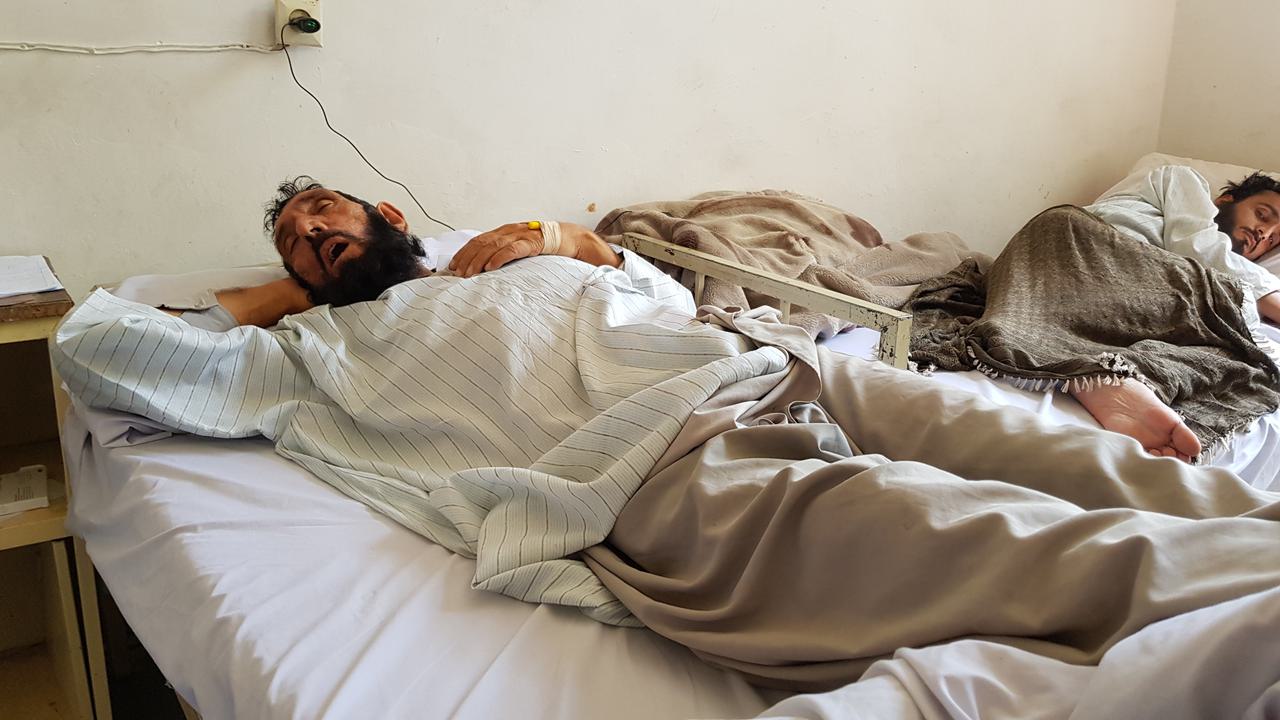
 Doctors at Mohmand hospital, Kandahar, report seeing patients die of superbug infections. Photo via Mohmand hospital
Doctors at Mohmand hospital, Kandahar, report seeing patients die of superbug infections. Photo via Mohmand hospital
Dr Niamatullah Lodin and Dr Younas Joyan, describe a typical case from April this year at Mohmand hospital in Kandahar, the country’s second biggest city. Mohmand is a glass-fronted private hospital which provides public healthcare free of charge during the month of Ramadan, and treats a surge of patients during this time as a result.
They said a 35-year-old woman was brought to hospital, unconscious and in a coma, by her family. She had given birth three days earlier and caught an infection. The bacteria had got into her bloodstream causing life-threatening septic shock. Lodin and Joyan gave her three antibiotics, ceftriaxone, vancomycin and metronidazole - but there was no improvement.
The two doctors checked her white blood cell count, an indicator of immune activity in response to microbes in the blood. A normal level is between 400 to 1,000. Hers was 19,000 and didn’t fall as expected after being given antibiotics. She had a severe and resistant infection.
The patient had lost a lot of blood after giving birth; her blood volume fell rapidly and her kidneys began to fail.
The doctors were forced to give her linezolid, an antibiotic only used for serious and resistant infections as it is toxic and can cause dangerous side effects. A long course will suppress the bone marrow, which will cause bleeding due to a low platelet count, anaemia due to a lack of red blood cells and increase the patient’s susceptibility to further infections due to a low white blood count. The drug is also poisonous to the kidneys and can cause severe skin rashes. Patients have died from the side effects.
“Giving linezolid to the patient was a difficult decision for us because it is a very strong antibiotic,” said Joyan, an internal medicine specialist, who gesticulated as he talked in a deep voice. “But when we saw her resistance against vancomycin and ceftriaxone we were obligated to give her linezolid, because it was the last option for us. If we didn’t give her linezolid she would have died.”
Fortunately this antibiotic worked; the woman’s pulse returned to normal and she started eating again. “The patient and her family were too pleased for what we did,” said Dr Lodin, a paediatric specialist at Mohmand. As the family was poor the hospital didn’t charge for care.
But not all patients that arrive at the hospital are so lucky.
Lodin and Joyan told the Bureau they see patients with drug resistant infections from streptococcus and klebsiella bacteria that have lost their lives.
‘We are also faced with patients who have been hospitalised for several weeks and even months because the infections are resistant to antibiotics,’ the doctors told the Bureau. They see patients with pneumonia, kidney infections and digestive system infections that do not respond to drugs. The most common multi-drug-resistant infections seen are from E.coli or TB bacteria, they said. It is estimated 1,400 people developed multi-drug-resistant tuberculosis in Afghanistan in 2016, according to the WHO, although only 138 were detected and treated.

Resistance rising
In Kabul, Afghanistan’s capital, Dr Mohammad Saber Hotak is head of pharmaceuticals at the public Antoni Infectious Disease Hospital. The hospital looks cramped and unclean. Very ill or unconscious patients lie in beds, their hospital gowns and sheets stained with fluids. It smells of vomit and illness. There is nowhere for families to sleep so they do so outside the hospital. Just one of the hospital’s two machines which show the results of a patient's full blood count, which is needed to diagnose certain infections or diseases and monitor the effects of treatment, is functional.
Hotak believes the number of multi-drug-resistant infections he has seen has increased by 20% in the past five years.
Around 150 patients a day are treated at the Antoni, many of whom are in very poor health. It deals with a daunting range of infections including rabies, meningitis, TB, malaria, typhoid, hepatitis A and E, yellow fever, anthrax, the bubonic plague, measles, chicken pox, polio and respiratory infections like pneumonia. It also has to contend with outbreaks of cholera seen in the country.
The hospital battles these contagious diseases with a very limited supply of medicine. It has basic supplies of antibiotics and fluids, but all other drugs have to be bought by the patients or their caretakers, usually from the pharmacy outside. This is the case in most hospitals in Afghanistan, while in developing countries patients hospitalised with infections rarely pay for drugs or supplies.
Around 15% of patients treated at the hospital have an antibiotic resistant infection. Hotak said most infections are resistant to ‘normal’ antibiotics and his teams are now seeing resistance to vancomycin, an antibiotic which is the last resort drug used to treat multi-drug-resistant bacteria. Two vancomycin-resistant superbugs - Staphylococcus aureus and Enterococci - are on the WHO’s list of bacteria for which new antibiotics are urgently needed.
Hotak, 48, has worked at the Antoni hospital for nearly 20 years. “That is due to other doctors not having the guts to work here due to the nature of the hospital, contagious diseases, and those of us who work here had to stay I guess,” he said.
“When you see a patient dying because of complications or resistance to drugs, it makes me feel sad that I couldn’t do anything to treat him or her," said Dr Mohammad Sadiq Naimi, head trainer and doctor at the Antoni hospital. “It has its negative impacts on the brain.”

The fuel for resistance
Overuse and misuse of antibiotics is the main factor fuelling resistance worldwide.
In Afghanistan, there is a strong cultural trend towards taking antibiotics, said Burtscher, of Doctors Without Borders. There is a belief that the dirty and dusty environment in the country causes ‘disease’ in the body, and that antibiotics are needed to ‘clean’ it. People take them for non-bacterial conditions, like colds or general body weakness, while women are given them after delivering a baby, she said. Patients travel for miles to buy drugs, and families stockpile them at home for when relatives get sick.
In addition, pharmacists do not always follow the regulations around prescribing the right drug or the full dose, which further fuels resistance. Patients are able to buy just one tablet of an antibiotic if they wish. Taking an incomplete course of antibiotics leads to resistant bacteria forming because it means the infection is not killed, and the most drug resistant bacteria survive and replicate.
There is also a problem with counterfeit and substandard antibiotics smuggled in from Pakistan or Iran. These contain either none of the active ingredient or less than the advertised dose, again fuelling resistance because a low dose means not all the bacteria will be killed by the drug, and the resistant ones will survive and spread.
The perception of substandard drugs can also cause doctors to prescribe higher amounts.

An unknown scale
Like most public hospitals in Afghanistan, Antoni does not have a formalised database to keep track of patients, their illnesses, or resistance patterns to antibiotics and so there is no empirical data to enable useful surveillance. Information is captured in handwritten books.
To find out how many patients have died, you would have to go through the notebooks one by one, Naimi said.
Similarly across Afghanistan nobody knows the scale of the superbug problem because there is no centralised system for recording the most common infections and their resistance patterns.
A handful of studies show an emergence of multi-drug-resistant bacteria in public hospitals, echoing trends across the Middle East. One study, from two public hospitals in Kabul, found 56% of Staphylococcus aureus bacteria were resistant to methicillin, the main drug used to fight it with the majority resistant to multiple drugs. Across the US the proportion is 46%, according to the US Centre for Disease Control and Prevention.
In order to quantify the problem you need a surveillance system, with laboratories equipped with the technology and staff to grow microbes and perform tests to see which antibiotics will work against them. Afghanistan has only 14 public microbiology labs in seven provinces. More labs are set to open this year, but even then, 20 out of 34 provinces will still have no access to public facilities.
Among the labs that do exist, the quality between public and private labs can vary, meaning doctors do not always send samples of a patient’s infection to a lab. “Some of them say ‘Oh, if I send a sample to the laboratory I don’t rely on the evidence’,” said Dr Safiullah Nadeeb, the WHO’s lead on AMR in Afghanistan. Stressed doctors are often also trying to treat 100 patients a day, and so don’t have time to send off for tests, he added. Nadeeb is trying to improve both infection control in Afghan hospitals and establish a surveillance system for resistant bacteria. The country has enrolled in WHO’s Global Antibiotic Surveillance System, where countries all around the world will submit data under the same protocols. Four sites in Afghanistan have been selected and will gather data to international standards. "Maybe by next year we will have very good data," Nadeeb said. Until then, “we are not able to report resistance and we are not able to address the issue."
Improving surveillance and infection control were two of the key changes made by the US army in its programme to reduce superbugs – a luxury civilian hospitals cannot imagine.

Finding solutions during war
The US military’s Antimicrobial Resistance Monitoring and Research programme (ARMoR), was launched in 2009.
Over six years doctors worked to lower resistance rates: improving hygiene and infection control; isolating patients when they came into hospital until they had been tested for drug resistance; introducing better record keeping around the antibiotics patients had previously received and reducing use of broad spectrum antibiotics. It started with an annual budget of a $1.5m, which doubled within a year. It spent an additional $6m on genetic testing of microbes, linking the results to clinical data.
While modest for the military, these resources are not available for public hospitals in Afghanistan, where implementing even low cost infection control measures is difficult.
“If you go to some hospitals and say why can’t you apply these measures of infection prevention they will say, ‘I don’t have chlorine. I don’t have gloves’,” said Nadeeb. Even in a top down, command-and-control system like the US military, it still took six years for improvements, some very basic, to take effect, said Liz Tayler, a technical expert on AMR with WHO.
“The fact that it still took so much time in a military setting shows what a tough time developing countries are going to have in tackling the problem,” she said.
Making the situation even tougher is 40 years of conflict.
While conflict continues, it is difficult to coordinate changes. Bawar said: “The mother of all disorganised systems is war, continuous war.”
Additional reporting by the Bureau's reporter in Kabul




