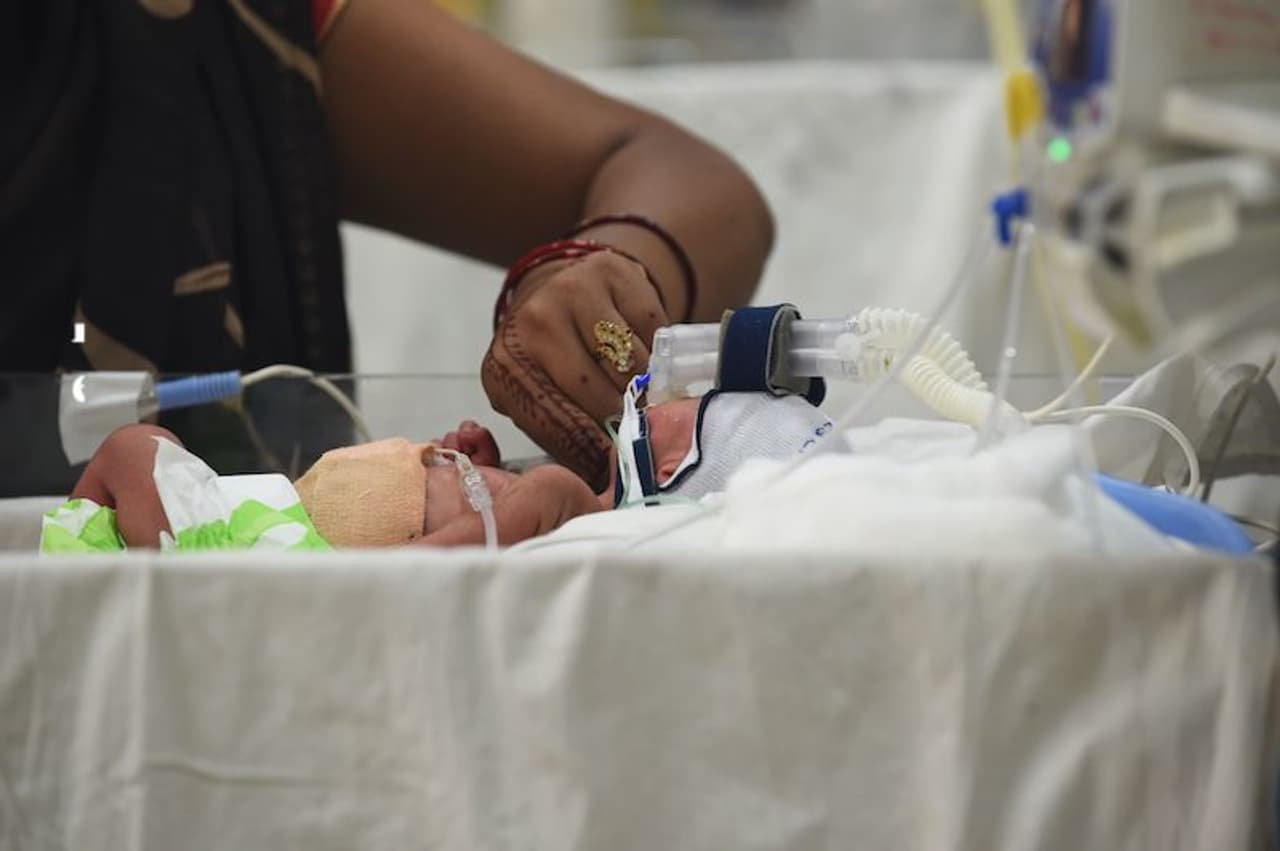
Babies hit the hardest by India's antibiotic resistance crisis
Baby Manu had been in the intensive care unit in the Indian city of Jaipur for 10 days with a life-threatening bloodstream infection. Her mother was extremely anxious, unable to feed or hold her child. As there was no window into the unit, she couldn’t even see her. Nobody was allowed into the ICU and Manu had to be cared for by one nurse, so the infection didn’t spread to other infants on the ward.
Manu was suffering from sepsis, a serious and potentially deadly condition where an infection gets into the bloodstream and the body overreacts. If left untreated, babies can go into septic shock and their organs can begin to shut down within hours. Manu had already been given powerful "last resort" antibiotics for more than a week. Perplexingly they didn’t seem to be working.
Laboratory tests came back revealing why. The infection that had spread to Manu’s blood was resistant to nearly every single antibiotic the hospital stocked, except for one: Polymyxin B. This explained why her infection hadn’t responded to the antibiotics she had already been given. Manu was given Polymyxin B immediately, but she had to be monitored carefully as it can damage the kidneys and nerves.
Babies less than a month old are vulnerable to catching infections as their immune systems have not developed yet, and if those infections get into the blood they cause sepsis. Globally, sepsis is one of the three leading causes of infant deaths. In India at least 640,000 babies died before they reached a month old in 2016, Unicef figures show.
Over the past decade hospitals have been faced with an extra threat. As was the case for Manu’s infection, they are seeing ‘alarming’ rates of antibiotic resistance in the types of bacteria that typically cause sepsis, making care of sick babies even more difficult. In most big city hospitals, where babies with sepsis are referred, common antibiotics are no longer effective. More than 80% of some types of bacteria causing sepsis in babies are multi-drug resistant - immune to nearly all antibiotics.
Doctors are having to administer "last-line" antibiotics, normally given only in emergencies, as the first drug. It was estimated in a study in 2016 that resistant infections kill more than 58,000 babies in India every year, though the author of the research said this was a vast underestimate.
"We are in a fix. We are staring at a gloomy situation," said Dr Suman Chaurasia, a paediatrician and sepsis researcher at the All India Institute of Medical Sciences, a top government hospital in Delhi.
Bacteria are becoming increasingly resistant even to these "last line" antibiotics. Older antibiotics, those not traditionally used for sepsis or combinations of drugs have been brought out to be used on adults with sepsis. But as there is a lack of data on how these options would affect a baby’s body, doctors cannot usually use these alternatives on infants.
“Our biggest concern is what kind of drug would be left for us?" said Dr Chaurasia. "If drugs like colistin are getting out of our reach, being snatched out of our hands, how are we going to treat babies further?”
“I can’t think of anything more threatening to mothers and babies' lives than antibiotic resistance,” said Professor Ramanan Laxminarayan, director of the Center for Disease Dynamics, Economics & Policy (CDDEP), a US public health organisation. “Antibiotics have made us lazy. It’s held out the hope that antibiotics will cure infection but they are working less and less often.”
He called for government policies to regulate sales and use of antibiotics and for better infection control in hospitals. “We are just not doing enough on infection control… We need hand washing, hand barriers against bacteria spreading. These are non-negotiable but they are flouted routinely in all facilities.”
India has become the global epicentre of antibiotic resistance, with many factors combining to hasten the spread of superbugs. Bacteria evolve resistance to antibiotics naturally over time, but the mass consumption of the drugs speeds it up dramatically, particularly if they are used inappropriately. India’s use of antibiotics in human medicine more than doubled between 2010 and 2015 as incomes rose. The country has a huge population, millions of whom are living in poor, unsanitary conditions, and there are frequent outbreaks of infectious disease which require antibiotics to treat.
Drugs are available over the counter and many people take the wrong antibiotics or an incomplete course; and a majority of people get medical care from unregulated private doctors who are often untrained and may prescribe inappropriately. This is combined with poor sanitation and infection control in many hospitals, allowing resistant organisms to spread.
Antibiotics have also been widely used in Indian farming to treat and prevent disease in cattle, chicken and pigs used for meat, milk and dairy. Tiny frequent doses are also used to fatten animals up for slaughter, a practice banned in the EU and US because this kind of use fuels resistance.
Finally the country is a global hub of antibiotic productions, and the pharmaceutical factories leak antibiotic-ridden effluent into the environment during the manufacturing process, as revealed in a previous Bureau investigation.
This “perfect storm” has led to soaring rates of resistance among bacteria in India, creating powerful superbugs which then spread all over the world. At three hospitals the Bureau visited in Delhi and Jaipur, there was a reported resistance rate to a group of last line antibiotics known as carbapenems of between 50 and 70%. In the UK fewer than 2% of bloodstream infections are resistant to these drugs.
It is having a huge impact on newborns vulnerable to infection, experts warn. Dr Chaurasia and his team produced a landmark study, tracking babies with sepsis from three government hospitals in Delhi. Before this, the lack of data meant sepsis was has not been taken seriously as a public health concern, he said.
His team found followed 13,530 babies between July 2011 and February 2014 and found nearly 15% suffered sepsis. They found the condition was responsible for nearly a quarter of all newborn deaths (in the UK it is responsible for less than 2%).
The levels of multidrug resistance was “alarming”, Dr Chaurasia said. One of the bacteria causing the sepsis, Acinetobacter, had a resistance rate of 82%. Two thirds of the babies infected with it died.
The study also found that most cases happened within the first three days of life, some within just 12 hours. It is very unusual for infections to be caught so soon and the doctors are not sure where they are coming from.
It could be that mothers were carrying bacteria and passed it to their baby in the womb, or in the birth canal during labour. Or it may be that unsanitary equipment or practises during pregnancy or birth introduced the bacteria to the mother and baby, such as unsterile forceps being used or staff failing to change their gloves or wash their hands between patients. The babies may also be catching the bacteria from the hospital surroundings or from doctors, nurses or families who visit.
After carrying out the groundbreaking study, Dr Chaurasia and his team hope to come up with solutions: alternatives to antibiotics that could be used on newborns, old antibiotics that could be repurposed, and if so, the dose that could be used. Currently there is no gold standard way to diagnose sepsis - sending a blood culture to a lab takes at least three days and a bacteria can’t always be grown. It is hoped a fast bedside test can be developed instead.
Some believe India should concentrate on improving the cleanliness of its hospitals. “Unless India improves sanitation in communities and infection control in hospitals we won’t be able to tackle antibiotic resistance at all,” said Dr Abdul Ghafur, a professor in infectious diseases and co-ordinator of the 2012 Chennai Declaration, a roadmap for combating antibiotic resistance in India.
Many are already working to improve infection control. The international NGO Jhpiego is working to lower rates of maternal and baby mortality by encouraging good menstrual hygiene, good birthing practices and appropriate antibiotic prescription in Indian hospitals, communities and families.
It can be difficult to instil these behaviour changes, said Dr Kailash Saran, head of Jhpiego Rajasthan. “We faced a lot of resistance from staff,” he said. “They assume the hygiene is poor so they give antibiotics… If we watch them they don’t prescribe but then they call the suppliers and get them to send antibiotics.”
Yet slowly, with mentorship and repetition, behaviours are beginning to change. “If you start explaining why you are doing certain things, people are more likely to follow,” said Dr Bulbul Sood, country director of Jhpiego India.
Two days after being given Polymyxin B, baby Manu seemed to respond. She was well enough to come off oxygen and be moved to a different ICU where her mother could visit and feed her breast milk using a tube. The family are now waiting, hoping she will recover.