
Disabled people trapped waiting years for vital home adaptations
As children, Rianna and Lauren Campbell-Thompson shared a bedroom. Lauren took the top bunk and Rianna, who has cerebral palsy and uses a wheelchair, took the bottom. Eventually Rianna moved to the room across the landing. It’s a distance of a few feet, but one Rianna cannot cross – the landing is too narrow for her wheelchair.
Rianna has not seen her twin’s room since about 2003. Instead, Lauren shows her photos.
A lift connects Rianna’s bedroom to the living room. But the rest of the three-bed terrace in Bromley that has been her family’s home for her entire life – the twins are now 28 – is cut off from her. She loves to bake, but cannot get inside the tiny kitchen because the doorway is tucked away in a corner. To wash in the wetroom, Rianna has to travel down in the lift naked before Lauren and their mum, Lorna Campbell, get her onto a shower trolley and wheel her inside. Then they must get her upstairs again to be dressed.
The family needs £100,000 to adapt the house into a proper home for Rianna. That money, Lauren said, would cover removing the lift and putting up a new wall to move Rianna’s bedroom downstairs, making the kitchen big enough for her to use and installing accessible equipment, and adding a new hoist.
In 2019 Lorna began an application for a disabled facilities grant (DFG) – the only grant available for home adaptations in England. It is a legal requirement for councils to financially support applicants who meet the DFG eligibility criteria, but there are limits to this support.
In England, the maximum amount councils can give each applicant is £30,000; in Wales, it’s £36,000; in Northern Ireland, £25,000. The cap has not been raised in England since 2008, despite recommendations four years ago to raise it to take account of inflation and “substantial changes to house prices, benefits, retirement ages”.
Lauren, who works as a part-time care worker, knew the grant would cover only a fraction of the cost of the work needed. She launched a £20,000 crowdfunding campaign and has poured years of effort into it for her sister’s sake. “It’s been quite hard to keep pushing on, especially finding ideas to help get the fundraiser moving … It’s quite embarrassing as well, especially showing the disrepair of the house, but it’s honestly the only way.”
And she knows she is not alone. “I have access to a lot of accessible housing pages on Facebook and everybody’s having to crowdfund the excess because with Brexit and inflation, everything’s gone up, but the DFG price hasn’t shifted. Most people’s quotes come in way over the £30,000 budget.”
 Rianna’s bedroom is one of only three rooms she can access at home
Alex Sturrock
Rianna’s bedroom is one of only three rooms she can access at home
Alex Sturrock
 Lauren shows her twin photos of her room since it’s not accessible
Lauren shows her twin photos of her room since it’s not accessible
In fact, nearly 80% of local authorities in England and Wales are using discretionary powers to top up funding, the Bureau of Investigative Journalism has found, after contacting every council in the UK for data on grants and waiting times. But the extra money a person can get varies wildly by council; some offer another £30,000 but Manchester can offer up to £70,000. In some areas, the top-up is a grant; in many, it is a loan.
Lorna still does not know if Rianna will be awarded a discretionary loan to top-up their grant of £12,000, which has been approved, after a long and sometimes fractious process. In May of last year, Lewisham council advised the family to manage the renovation project themselves, despite their inexperience. It adds to Lorna’s worries, after two physically and mentally draining years.
Lauren is equally disheartened and disappointed. “It's not fair. I've spoken to one woman who waited five years for a DFG. She was showering in the garden with a garden hose. Lots of people get left behind and I think a lot of people are going to die, especially now with rising living and energy costs. Rianna’s got a bad situation, but there’s people in worse situations, and they don’t have people like me or mum to do the process for them, or stick up for them.”
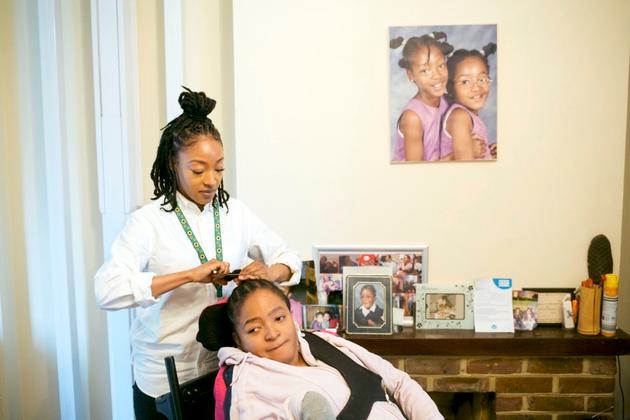 Lauren brushes Rianna’s hair in the living room of their home
Alex Sturrock
Lauren brushes Rianna’s hair in the living room of their home
Alex Sturrock
The DFG application process is supposed to take a maximum of 18 months – six months to approve, and a year to complete the work. It is a long time to be without vital necessities: an accessible kitchen, a safe place to wash, a way in and out of your home.
However the Bureau has found that the true waiting time can stretch even longer, because before a disabled person or their relative can even apply, their needs have to be assessed by an occupational therapist. Without their sign off, there’s no hope of even applying for a grant.
Fazilet Hadi, head of policy at Disability Rights UK, said: “The current delays in the system are having a devastating impact on the lives of Disabled people and their families. Most people take bathing, cooking, and other everyday activities for granted, yet we are making Disabled people wait months and years for basic changes to our homes, which would enable us to live independently and safely.”
After fighting for years to secure adaptations for her sister, Lauren faces an uphill battle to get an assessment for her own hidden disabilities, including autism and ADHD. The grant could pay for soundproofing in her front bedroom, converting the garage into a bedroom, or providing more space for Lauren and her service dog, Harley. Despite her experience with the system, she did not realise she was eligible for a grant until fairly recently. But she quickly hit a roadblock; Lewisham council told her it had no specialist occupational therapists who could assess non-physical disabilities. Until she gets assessed, she’s stuck.
Lewisham council said it had suggested the family manage the adaptations themselves because the family had expressed a lack of confidence in council staff in the past, but told us: “Council staff have a duty to advise and support the family through the process and are more than happy to do so.”
Many parents of autistic children told the Bureau there was a lack of specialist knowledge to assess home adaptations for their particular needs. In February the Labour MP for Leeds Hilary Benn raised a question in parliament on the issue, emphasising the need to keep children in their own homes.
‘Be prepared to wait’
In a first of its kind analysis, the Bureau has found long and growing waits for occupational therapist visits that are forcing thousands of disabled people to sacrifice their independence and dignity for years, while others are trapped inside or locked out of their own homes.
In nine council areas in England and Wales, people had to wait on average more than a year to see an occupational therapist and complete the pre-application steps, including Southend, where the wait is more than 18 months.
Government rules mandate that adaptations are approved and completed within 18 months, meaning a person could easily be waiting two to three years for the changes that make their house a liveable home. Councils only have to record the average waiting times, so many are likely waiting longer. Indeed, some areas in Northern Ireland, where grant rules are different, had wait times of more than three years.
The difference in response times across England and Wales was stark. In some places in Wales – such as Cardiff and Conwy – the average wait for an occupational therapist was barely a few days, but in Newport it could be up to a year.
Kate Sheehan, who has worked as an occupational therapist for 35 years, told the Bureau the pandemic had worsened the backlog, but shortages had been apparent even before Covid-19. She said: “I think the lack of bursary has an impact. Historically, the health authorities funded places and then, of course, the bursaries went, which meant that even if you were passionate about occupational therapy, you were paying £9,000 a year fees. And to be brutally honest, the pay scale is not great in social care and the NHS.”
Several councils told the Bureau they were struggling to recruit and train enough therapists to provide quick assessments. The cancellation of a visa programme that let overseas foreign therapists “plug the gap”, particularly in places like London that had also hit hard, Sheehan added.
It is no surprise that many people turn to fundraising or family rather than wait months to have access to their own homes. Phill Thompson believes he would have ended up in a care home, at the age of 36, if his father had not given him tens of thousands of pounds from his savings after a catastrophic motorcycle accident that left him with a spinal injury.
His community occupational therapist said there would be nobody available to assess his home for adaptations until a few months after leaving hospital. All he was offered was a bed and a commode, and the suggestion he live in one room.
“If we hadn't had the ramp done, I wouldn't even have been able to go in and out of the house,” he said. “Be prepared to wait and don’t hold your breath. Sure, it'll happen, ultimately. But you’re just going to have to wait. And good luck, I hope you enjoy living in one room downstairs in your house, not being able to have a bath or shower.”
Across the country in Fareham, Hampshire, Derek Biggs is living the future Thompson feared – stuck in a residential care home, not because he needs to be there, but because his home has not been adapted for his needs. He has paraplegia and was discharged into the care home after a recent hospital stay, but when he later applied for a grant he was denied on the grounds his savings and his son’s income could pay for the changes.
A second assessment found he needed many more adaptations to let him come home, costing up to £70,000. The only financially sound option for the Biggs family is to move – but finding a property that suits their needs is hard work.
At the heart of the housing crisis for disabled people is a historic lack of accessible properties across the UK. The 2021 national disability strategy acknowledges that “less than half of the local plans in England for new homes include requirements for a proportion of new homes to meet higher accessibility standards”.
Until they can find a large enough bungalow, Derek has to stay at the care home, where he cannot receive rehabilitative care. “There’s a lot more to the rehab than just getting up and sitting in the chair – to be independent anyway,” he said. “I can always get people to push me around, but I’m not that sort, you know? I’ve never allowed anybody to push me around in the wheelchair.”
Fareham council said it was not able to disclose the financial details surrounding Derek’s grant, but told us he was “one of the first beneficiaries” of an update to its policy last summer that allowed the council to offer him a discretionary grant.
Christina McGill, interim director of strategy and external affairs at Habinteg, a housing association that has prioritised accessible homes, said: “Just 9% of homes in England provide even the most basic accessibility features. That’s why Habinteg is calling for changes to building regulations to lift up the minimum requirement to the ‘accessible and adaptable’ standard and for all local plans to require a percentage of new homes to be designed to meet the daily living needs of wheelchair users.”
A tale of two councils
Lisa Parker first found out about disabled facilities grants in an autism support group on Facebook; her twin boys, Michael and Jaxon, have autism and a rare chromosome disorder, and her younger son Blake is also being assessed for autism.
But it was not just her own home she thought of. Her father, Peter Gilroy, has a prosthetic leg but has to use a wheelchair if he wants to cook, as his oven is too low to be used while standing up. Instead he must remove his prosthetic leg, wheel himself into the kitchen, get off his wheelchair, bend down on one knee and balance as he takes out hot food and reaches up to put it on the surface. Before he can eat, it’s back to the bedroom to put on his leg again.
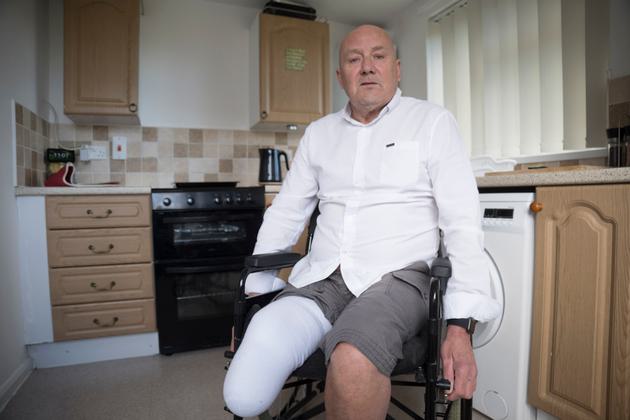 Peter has to remove his prosthetic leg if he wants to cook ...
Mark Pinder
Peter has to remove his prosthetic leg if he wants to cook ...
Mark Pinder
 the oven is too low to be used while standing up
the oven is too low to be used while standing up
He was left waiting for a visit from an occupational therapist to discuss kitchen renovations for at least four months. In the meantime, a council worker told Lisa he could live off microwave ready meals.
She was outraged. “He has to have a healthy, balanced diet. He’s been diabetic for 23 years and now he’s 67, he’s been told he’s got to live off microwave meals. It’s not good enough … I said to dad, ‘you can’t live like this. It’s not fair.’”
Sunderland council told us the “health and wellbeing of the vulnerable is always a priority”, but referred to the pressures of the pandemic, as well as local and national pressures on adult social care services. After the Bureau contacted the council, Peter was visited by an occupational therapist and has been told that he can expect his kitchen to be adapted within the next six months.
However, just a 25-minute drive away, Lisa’s grant from South Tyneside council has transformed the home for her sons. “Their behaviours are challenging and they’ve got a communication disorder as well, so communicating is quite difficult,” she said. “Their needs are all very different. Michael’s more of a stronger person in personality. He’s quite loud and physical. Whereas Jaxon’s a little calmer and not so physical. And Blake is just in his own little world.”
The family has been awarded the maximum £30,000 per child, which has so far funded wall padding – “Michael tends to kick, body bang and head bang on that wall” – stable doors and patio doors for easier access to the garden in their privately rented home. A loft conversion and changes to the garden are to come.
“They’re going to put astroturf down the full size of the garden because it’s easier and are going to remove the stones because they’re a choking hazard for the boys – they chew and mouth everything. The garden doors are in and we are so happy with them. The boys were very excited when they saw them and they’ve had loads of time in the garden.”
Adaptations like these for people with sensory needs or who are neurodivergent are rarely mentioned in literature around disabled facilities grants. Lisa told the Bureau: “Straight away I went on Gov.uk. There’s a lot of information on there, although it’s very basic. It certainly doesn’t cover what we’re getting.”
 Peter smiles as his grandson plays in his wheelchair
Mark Pinder
Peter smiles as his grandson plays in his wheelchair
Mark Pinder
The Department for Levelling Up, Housing and Communities said: “It is vital disabled people are fully supported with adaptations and improvements, so they are comfortable and secure in their homes. Since 2010, we have provided councils with more than £4bn to deliver around half a million home adaptations and an expert body is on hand to help any council reduce backlogs, so older and disabled people can live independently and safely.
“We appreciate the challenges councils have faced to deliver these grants during the pandemic, but it is now crucial that adaptations are delivered at pace and the backlog on waiting lists reduced.”
Updated guidance for English councils delivering grants effectively was finally published in March. It outlines “best practice targets” for all stages of the process, including before an application is submitted, and says the timescales “should be met in 95% of cases”. However, a promised public consultation on significant reforms has yet to materialise.
The Welsh government said it had given an extra £1m to local authorities last year for adaptations and planned to increase it again this year.
Experts want the grants to be both more efficient and more widely promoted, particularly to Black and minority ethnic communities. Along with building more accessible homes, these improvements would raise the standard of housing and therefore, health outcomes, for those who spend the majority of their time indoors.
Get involved
Want to investigate this story in your area? Use our reporting recipe to dig into the local data
Find out moreAmanda Batten, chief executive of the disability charity Contact, said: “We need more accessible social housing, particularly larger properties and suitable supported housing for disabled young people. We believe greater priority should be given to families with disabled children for social housing.”
Sheila Mackintosh, a housing consultant who led the 2018 review of disabled facilities grants, believes there is a will across the sector to improve. “The people working in the field of home adaptations are some of the most caring and committed people you will meet. Everyone is doing their best. There are some excellent services and a lot of very satisfied customers. People should not be deterred from coming forward to get help.”
Despite the difficulties she’s had helping her father, Lisa also encourages anyone who needs it to take advantage of the grant scheme. On her Instagram account she offers help and support to other people in need of adaptations to live with independence and dignity.
She said: “If you had no food in your house, and you needed to feed your children, you’d go out there and do anything you can to bring a meal to the table. It’s the same. We’re a family with children with disabilities, if they need that extra room or whatever, you know, do it. Don’t give up.”
Header image: Lauren Campbell-Thompson helps twin sister Rianna into the bathroom of their Bromley home. Credit: Alex Sturrock
Reporting team: Vicky Gayle, Rachel Hamada, Charles Boutaud and Ioana Cerasella Chis
Community organiser: Emiliano Mellino
Bureau Local editor: Emily Wilson
Editor: Meirion Jones
Production editor: Frankie Goodway and Emily Goddard
Fact checker: Alice Milliken
Data table made with Flourish
Our reporting on health inequality is part of our Bureau Local project, which has many funders. None of our funders have any influence over the Bureau’s editorial decisions or output.
-
Area:
-
Subject:





