
How superbug-infected pigs get into Britain unchecked
Pigs infected with the superbug MRSA can be freely imported into the UK due to regulatory loopholes, the Bureau can reveal.
An investigation has established that there is no mandatory screening for live breeding pigs leaving Denmark – where MRSA is rife throughout the country’s herd – and entering the UK.
Experts are warning that if no action is taken, the UK’s pig herd could rapidly become infected. Such an epidemic could have a serious impact on human health, according to leading Danish microbiologist and MRSA expert, Professor Hans Jørn Kolmos. Thousands of people have contracted the livestock-associated strain of MRSA in Denmark and six have died from it in the last five years.
The Bureau has established that at least one regular Danish supplier of pigs to England was contaminated with the bug in 2014. This supplier exported 41 pigs to England in the last three months.
Our investigation has also confirmed that British-produced pork contaminated with livestock-associated MRSA has already made its way onto the shelves of major UK supermarkets Sainsbury’s and Asda – and three cases of the superbug in humans have already been recorded in this country.
New tests discovered three packets of supermarket meat contained a livestock variant of MRSA that is resistant to a range of antibiotics, including medicines that are critically important in human healthcare.
If left unchecked LA-MRSA could turn into a major problem for the UK, warned MP Kerry McCarthy, who has been campaigning on the issue and is “alarmed” by studies showing the bug is likely to become well-established in the British pig herd. “The Government must act now to avert this public health crisis,” she said.
The strain that affects pigs is known as Livestock Associated Methycillin Resistant Streptococcus Aureus (LA-MRSA) CC398. It can be passed to humans when they work directly with infected livestock – the primary transmission route – but also when they handle contaminated meat.
The disease is resistant to human medicine. While many people can carry the bacterium without getting ill, LA-MRSA CC398 can cause skin complaints as well as more serious and life-threatening infections – mainly in people with underlying conditions such as pneumonia and blood poisoning.
UK public health chiefs say it does not pose a significant risk to human health because the bacterium is killed when meat is properly cooked. But in Denmark, which has a population 11 times smaller than Britain, up to 12,000 people are estimated to have contracted CC398 in the past decade – though the real figure could be higher.
Denmark should serve as a warning of what could easily happen in Britain, say experts.
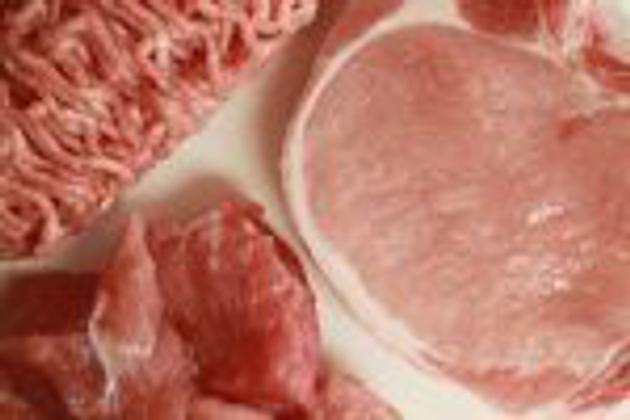 Livestock-assisted MRSA has entered the domestic food chain (Photo by Sean Gallup/Getty Images)
Livestock-assisted MRSA has entered the domestic food chain (Photo by Sean Gallup/Getty Images)
Aside from the threat to human health, there are concerns about the potential impact on pig farming, a sector that is already under severe financial pressure.The British herd is thought to be largely free of MRSA, as was Denmark’s less than ten years ago. Today as many as two thirds of the Danish herd are estimated to carry the bug – yet the country remains one of the European Union’s (EU) main exporters of pork and live breeding pigs.
The Bureau has seen the results of testing carried out on 97 samples of British-produced pork sold in UK supermarkets, carried out by the campaign group Alliance to Save Our Antibiotics, which found CC398 in three packets of meat. It tested samples from Asda, Aldi, Co-op, Morrisons, Sainsbury’s, Tesco and Waitrose, and found the superbug in British-produced pork mince from Asda in Northamptonshire and Bristol and Sainsbury’s in Surrey.
The bacterium found in all three mince packets was fully resistant to tetracyclines, a group of antibiotics which are among the most widely-used in intensive pig farming and are also used to treat urinary tract and sexually transmitted infections in humans.
The Sainsbury’s sample was also resistant to fluoroquinolones and trimethoprim, also both widely-used in pig farming as well as human medicine. The Asda samples were partially resistant to flouroquinolones and were fully resistant to macrolide and lincosamide antibiotics – again common in pig farming and human medicine.
“It is extremely worrying to find LA-MRSA in British-produced pork,” said Alliance spokeswoman Emma Rose. “Scientists are now warning that the extensive (MRSA) reservoir in animals could ultimately lead to a pandemic spread in the human population. LA-MRSA is able to cause serious and potentially fatal infections in humans, and as the bacteria is resistant to antibiotics, it is extremely difficult to treat. What’s more – even more dangerous variations are emerging as the superbug evolves.”
CC398 was first identified in livestock in the Netherlands in 2004. Since then, it has spread across Europe, infecting farm animals and people. The infection has been found in cattle, horses, chickens and turkeys, but pigs are the primary species affected.
The superbug has been linked to an overuse of antibiotics in factory farming – where often cramped and dirty conditions allow disease to flourish, and farmers can become reliant on drugs to keep animals healthy.
CC398 is one of a growing number of antibiotic resistant superbugs. The growth of antimicrobial resistance (AMR) – referring to bacteria becoming immune to commonly-used antibiotics – poses a grave danger to global public health. The NHS’s chief medical officer Dame Sally Davies has described antibiotic resistance as posing a “bigger threat than terrorism” – while a major global review by economist Lord Jim O’Neill earlier this year predicted resistant superbugs would kill more people than cancer by 2050.
The Bureau has identified several gaps in regulation which mean LA-MRSA is able to spread to the British pig herd. Firstly, while Denmark says it has one of the world’s most comprehensive pig health screening systems, producers are not legally required to screen export animals for CC398. Livestock known to be infected can be freely exported.
The next issue arises in Britain. While imported pigs must be guaranteed to be free from a number of diseases, this strain of MRSA is not one of them. This is because CC398 is not classified as a notifiable disease by Public Health England.
Since first being found in Danish pigs in 2006, CC398 has travelled well beyond the confines of farms, spread by agricultural workers or through contaminated meat. The variant is now estimated to account for about 40% of all human MRSA cases in the country.
 Intensive farming encourages antibiotic resistance (Photo by Josep Lago/AFP/Getty Images)
Intensive farming encourages antibiotic resistance (Photo by Josep Lago/AFP/Getty Images)
More than 600 people were known to have contracted CC398 in Denmark in 2013. The following year 1,276 cases were recorded, while last year another 1,172 cases were confirmed, according to government figures.
In some cases CC398 proves fatal: since robust screening procedures of humans were introduced in Denmark in 2012, six people are known to have died after contracting it.
Newborn babies have also been found carrying the bug, transmitted from their mothers.
Last year the Danish government announced a major plan to tackle the rates of CC398 by reducing the amount of antibiotics used in pig production by 15% by 2018.
It also announced plans to improve biosecurity on farms, through measures such as improvements of pig farm workers’ hygiene and programs to monitor the development of MRSA.
But the initiative did not include mandatory screening of breeding pigs destined for export markets.
Professor Kolmos said the strategy had major deficiencies. “The plan takes no actions against trade of live MRSA positive pigs, knowing well that this – according to scientific studies – is the most important way to spread MRSA,” he said. “If [Britain is] to avoid the problems we have [in Denmark] with pig-associated MRSA, you have to stop the import of live MRSA-positive pigs as soon as you can.”
The most recent Danish trade figures available show the UK imported more than 3,000 Danish breeding pigs in the past six years, including 916 animals in 2013, 598 the year after and 283 in 2015.
In July 2014, Britain’s first confirmed case of CC398 in a pig farm was identified: in Northern Ireland, a single piglet was found to be infected after being sent for post-mortem. Although the animal died of pneumonia, MRSA was found in its liver, lungs and spleen, according to an industry publication.
In January 2015, two more piglets originating from a separate farm in eastern England were found to be infected – they were submitted to a government laboratory for post-mortem after showing signs of skin disease. In total, 60 pigs from the breeding farm showed symptoms of illness, and six died as a result of the disease.
Upon questioning Public Health England (PHE), the Bureau discovered three confirmed human cases of CC398 had been recorded in the UK. None of the cases were linked to people working in pig farming, raising concerns the infection was spread by contaminated meat or already exists in the human community. PHE would not release details of where or when the cases were diagnosed as the small number of cases meant to do so would risk identifying the people involved.
Although veterinary health officials have declined to speculate about the origins of the outbreaks in pig farms, industry publications reported that imported animals were believed to be responsible for the case in Northern Ireland.
What exactly was found in British supermarket pork?
Multi-locus sequencing typing – a type of testing considered the “gold-standard” for identifying specific strains of bacteria – was carried out by the Alliance to Save Our Antibiotics on 97 samples of pork products from major British supermarkets.
Three packets of pork mince – two from Asda, one from Sainsbury’s – were found to contain LA-MRSA CC398. A Guardian Films investigation last year revealed imported Danish meat had been contaminated with the superbug – but this is the first time individual British supermarkets have been named in relation to UK-produced pork.
The bacterium in all three packets were tetracycline-resistant. Tetracyclines are the most widely used antibiotics in intensive pig farming and are used to treat urinary tract and sexually transmitted infections in humans.
The pork from Sainsbury’s was also fluoroquinolone-resistant. Fluoroquinolones are a class of antibiotics used in pig farming, which in human medicine treat respiratory and urinary tract infections.
It was also resistant to trimethoprim, an antibiotic widely use in farming, which is used to treat bladder, lung, middle ear infections and traveller’s diarrhoea in human medicine.
While the samples from ASDA were not fully fluoroquinolone-resistant, they showed intermediate-level resistance to the drugs.
They were also resistant to macrolide and lincosamide antibiotics. Macrolides are very widely used in pig farming, and lincosamides are quite widely used too.
Macrolides are prescribed for respiratory, skin, soft tissue and sexually transmitted infections in humans, while lincosamides are used to treat a range of bacterial infections.
The Bureau has learnt that at least one major Danish pig-breeding company that supplies animals to England – Breeding Centre Rønshauge A/S – has been contaminated with CC398 in the past. The company operates three pig-breeding facilities, and claims on its website to regularly supply both live pigs and semen to more than 30 countries – including England – as well as to clients in Denmark itself.
Rønshauge says it has more than 750 breeding animals in artificial insemination stations globally, and claims that as many as one in four Danish pigs carry the company’s pig genes.
Rønshauge pigs tested positive for CC398 in 2014 during government sampling, according to a list of more than 200 Danish pig farms found to be infected with LA-MRSA during official testing carried out between 2011 and 2015.
The official Danish export database shows Rønshauge exported 16 pigs to the UK in December 2012, 65 in March 2013 and 41 in July this year.
The Bureau also established that another pig breeding firm supplied by Rønshauge was found to be contaminated with CC398 during the testing. The company, Solvang Swineavl, is a large exporter of breeding pigs in its own right with international customers in Belgium, Italy, China and Brazil.
The data was published for the first time earlier this year by the media organisation Investigative Reporting Denmark following a lengthy legal battle.
Farming bodies tried to prevent publication of the list, arguing that it could prove detrimental to the individual farmers named and the industry as a whole. Until January the authorities had refused to publish it, only doing so after Denmark’s highest court ruled against the ongoing secrecy.
Rønshauge declined to answer questions from the Bureau about the number of animals it had exported to the UK in recent years, or whether it voluntarily screened its animals for CC398. The MRSA strain was prevalent in many EU countries, it said, so it was no surprise it was present in some Danish pigs.
It did not comment on its current MRSA status, but said: “In both production and export of pigs we follow – as any other Danish producer – all the rules from European and Danish authorities.”
Tim Petersen, from the Danish Ministry of Environment and Food, said that the official MRSA screening tests should only be seen as “snapshots” of specific farms and places where animals were tested. But he admitted that there were “no screening procedures in place neither in the EU nor in Denmark by which the farms [or] herds can declare themselves free after being found infected.”
How gaps in enforcement could help spread of superbug
Animal health officials do not have the necessary legal powers to contain LA-MRSA CC398 even after outbreaks are confirmed, a government contingency planning document reveals.
According to the document, current policies allow officials to carry out laboratory surveillance of the bacteria concerned and to access premises and livestock for sampling. Yet “additional policy tools” – such as putting movement restrictions on livestock, restricting the disposal of farm waste, slaughtering animals and restricting the prescription and supply of antibiotics – are “not currently available because the legal powers are not in place”.
This potentially hampers efforts to contain disease outbreaks: “Taking the first three bullet points together [movement restrictions; disposal of farm waste; slaughter], the advantages would be achievement of a much closer control of the situation on affected premises,” the document states. “The risk of dissemination of the resistant organism (from that premises) could be much reduced.”
Notifiable diseases – such as salmonella – are subject to stricter control, the document notes, than non-notifiable illnesses such as LA-MRSA.
The Veterinary Medicines Directorate said that while the spread of CC398 is not controlled through restrictions on movement, they continued to work with industry and stakeholder groups to tackle the issue, including developing specific guidance on improving biosecurity.
“The fact that LA-MRSA is not a notifiable disease does not affect our ability to identify LA-MRSA through clinical surveillance programmes and research run by UK government,” a spokesperson said.
Separate documents obtained by the Bureau reveal officials investigating England’s first pig related CC398 outbreak in January 2015 were hindered by a farmer’s refusal to allow detailed sampling at the breeding facility believed to be at the centre of the outbreak.
Officials discussed invoking statutory powers in order to gain entry to the farm, but were worried that such action might jeopardise voluntary sample submissions in the future. The consensus was that “there was no appetite to enforce further testing (using legal powers) on the farm.”
A spokesperson from the Animal and Plant Health Agency confirmed that three cases of LA-MRSA had been found in the UK by January 2015 – one in pigs in England, one in pigs in Northern Ireland and one in poultry in England – but said the official response was considered “appropriate and proportionate to the risk.”
The body declined to confirm whether any sampling was subsequently carried out, or whether further farm visits were made.
Campaigners describe the lack of enforcement measures as “worrying” and say wider surveillance is needed: “The current controls are inadequate, in large part due to the lack of appropriate surveillance and testing [which are] crucial to determining the extent of the LA-MRSA problem and to helping define the measures required to contain and control it,” said Emma Rose, from the Alliance to Save Our Antibiotics.
Alliance spokeswoman Rose said it was astonishing that no active government screening of the British pig herd for LA-MRSA had occurred since 2009 – when an EU wide survey was carried out and no MRSA was found in UK farms – despite repeated calls for testing.
As such, it was impossible to know how many pigs were infected and what the potential risk was to public health.
“If we are to have any chance of heading off this catastrophe, the government needs to put in place some basic measures to tackle the spread of LA-MRSA,” she said. “The systematic overuse of antibiotics on intensive pig farms – which is strongly linked to the emergence of CC398 – must stop.”
Professor Erik Millstone, a food safety expert at the University of Sussex, said the FSA was wrong to downplay the seriousness of LA-MRSA.
“The FSA might give its usual response of: ‘If people cook food properly then they’re not at risk’,” he said. “But not everyone cooks everything properly, and cooks often handle [meat] before they cook it. We increasingly eat outside of our homes, and from kitchens in cafes and restaurants where it’s impossible for consumers to know how the food is prepared or cooked.” People could also get the infection from those working at farms and slaughterhouses, he added.
“The emergence of antibiotic strains of pathogenic bacteria is a huge threat to human health and the health of livestock,” he said.
The National Pig Association (NPA) has developed its own voluntary protocol for pig farmers and breeders to try to stop the growth of CC398 in the British pig herd. It focuses on the entry point – infected pigs from other countries arriving in the UK.
The Red Tractor certification scheme – to which more than 90% of UK pig producers are signed up, requires importers to ensure the stock they buy has been tested for the bug in the source country, whenever a new supplier is used. Regular testing must then continue.
Neither the NPA nor Red Tractor would confirm whether they held data on compliance levels for the protocol however, or data on the number of pigs found to be infected with LA-MRSA.
David Clarke, chief executive of Red Tractor, admitted there had been procedural failings in the past but said this would not be acceptable going forward.
He told the Bureau: “Going forward we intend to enhance the Red Tractor standard to require specific veterinary checks on the pathogen test results of every consignment and we will expect to see a signed veterinary certificate of disease-free status.”
Sainsbury’s said it believed LA-MRSA was “very uncommon” in British pork and it always advised customers on how to cook meat properly and use basic kitchen hygiene.
It said in a statement: “We only allow the use of medicines on farm for animal health and welfare purposes, and under the strict supervision of a vet. We work closely with our farmers to ensure antibiotics are used responsibly and are taking advice from leading industry experts on this issue.”
Asda said: “Our customers can be assured that we are working closely with industry groups and farmers to make sure that antibiotics are used responsibly in farm animals.”
A Department for Environment, Food and Rural Affairs (Defra) spokesperson said: “Livestock-Associated MRSA is not the same as MRSA strains that can cause healthcare-associated infections and if meat is handled and prepared properly, the risk to people is low.
“Defra and the National Pig Association recommend that pigs imported to Britain are screened for LA-MRSA. The Government is currently reviewing options for surveillance, which will be proportionate to the very low health risk posed by Livestock-Associated MRSA.
“Tackling resistance to antibiotics is one of the Government’s top priorities. We are already making good progress in the UK and have set out a clear commitment to significantly reduce the level of antibiotic use in livestock.”
Zoe Davies of the NPA said: “Presence of resistance to antibiotics in LA-MRSA cannot be directly attributed to malpractice in use of antibiotics in the country where it is detected, since LA-MRSA retains the resistance genes even when the bacteria may not have been exposed to the antibiotic.
She said that Dutch and Danish farms have a high prevalence of LA-MRSA even though significant reductions in antibiotic use in farming have been made.
“There is no specific UK or EU legislation for the control of MRSA in companion animals or livestock. Government is constantly reviewing the range of surveillance and control options available for new and emerging disease situations, including those involving AMR, but clearly such measures must be demonstrably proportionate to the risk to human and animal health. LA-MRSA is considered to be of low risk to public and animal health and it is not a food safety concern.
Get all of TBIJ’s antibiotic resistance updates on Twitter: @TBIJAntibiotics


