Use of ‘last hope’ antibiotic soaring in English hospitals
Experts say a rise in the most dangerous types of superbugs is to blame.
Use of the ‘last hope’ antibiotic colistin - one of the few options left that can save lives when infections have become resistant to all other drugs - has soared in English hospitals, with experts blaming a rise in superbugs.
Prescriptions of colistin, which doctors use when infections stop responding to all other antibiotics, rose by 40% between 2014 and 2015, show figures obtained by the Bureau of Investigative Journalism.
It is a clear indication that multi-drug-resistant superbugs are becoming more and more common, say medical experts. But the increased usage of colistin means it’s only a matter of time before it stops working too - which would have dire consequences for human health.
Colistin is so important that regulators around the world have recommended its usage on animals be slashed, because overuse of antibiotics in agriculture is one of the prime ways bacteria develop resistance to the drugs. Yet the Bureau has learnt the government licensed three new colistin products for use on British farms last year.
Such a move was “sheer, utter madness”, said Professor Timothy Walsh, one of the scientists who originally discovered colistin resistance.
Colistin resistance has already been detected in various parts of the world - in one recent case, a 70-year-old woman died from septic shock in Nevada, after tests showed 26 antibiotics - including colistin - could not have stemmed her bloodstream infection.
Resistance will spread "as sure as eggs is eggs"
Such resistance is still extremely rare; however if current prescription rates continue then colistin resistance will spread in England “as sure as eggs is eggs,” said Dr Michael Weinbren, a consultant in infectious diseases and infection prevention and control at Chesterfield Royal Hospital NHS Foundation Trust. “You’ve got to be terrified and we need to be doing something about this,” he warned.
The term superbug refers to an infection which has become resistant to the antibiotics usually used to treat it. Some superbugs have become resistant to virtually all antibiotics, and genes and enzymes have now developed which can turn bacteria found naturally in our gut into resistant superbugs.
The steep rise in antibiotic resistance is now considered one of the gravest public health crises facing the world; without antibiotics, many infections would become fatal and routine operations would be too risky to carry out.
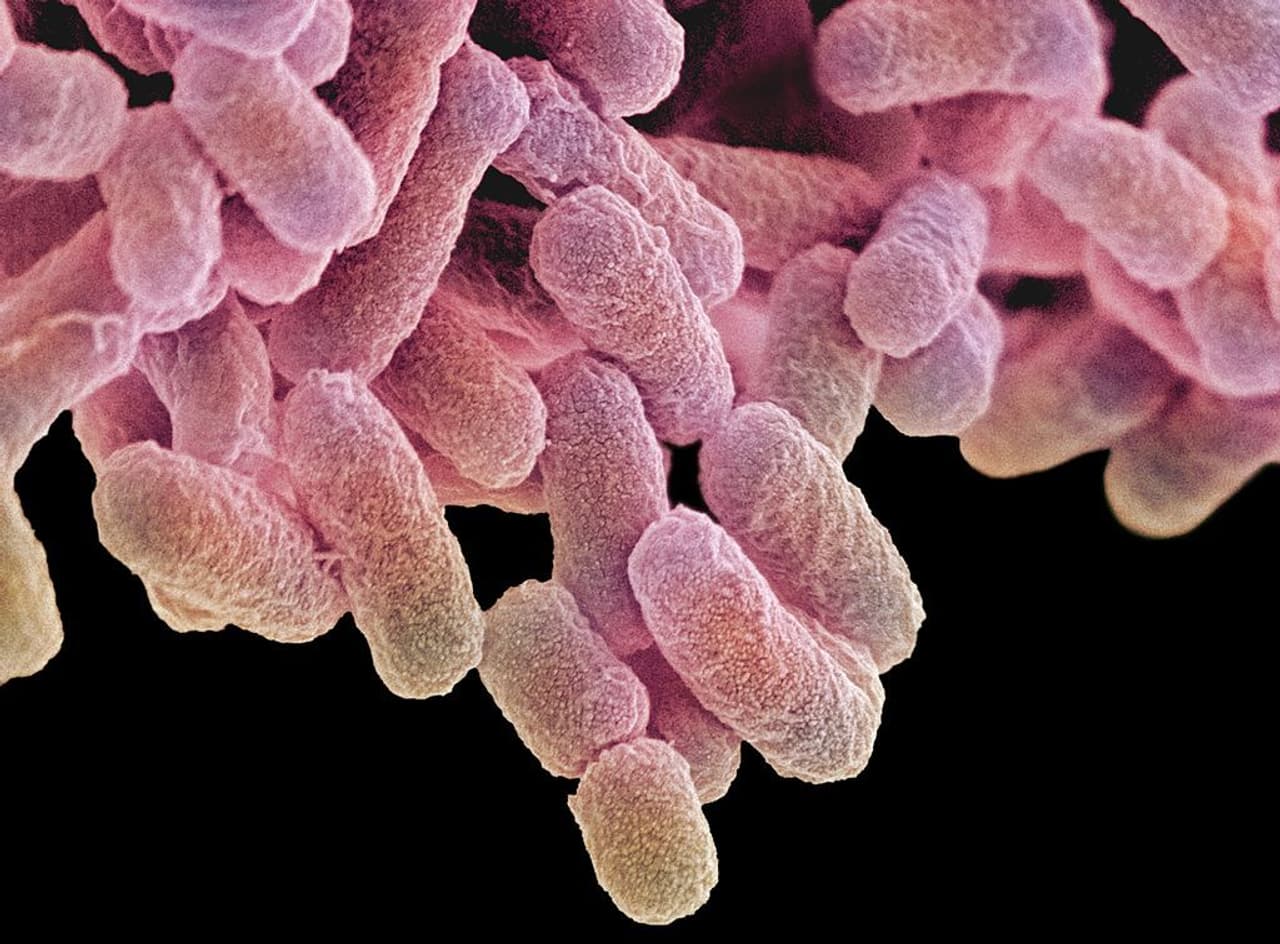
A group of antibiotics known as carbapenems are currently used as a last ditch treatment for superbugs which aren’t affected by other medicines. This family of bugs, known as carbapenem-resistant Enterobacteriaceae (CRE), includes evolved versions of common bacteria such as E.Coli and Klebsiella.
Epidemiologists have called CRE ‘the nightmare bacteria’ because 40 to 50% of people who suffer a bloodstream infection from them die. When a patient gets a CRE infection, colistin is one of few options doctors have left that has a chance of working.
Data sent to Public Health England and obtained by the Bureau reveals defined daily doses of colistin - the average dose a day for an adult when the medicine is used for its main purpose – rose by 40% from 346,143 to 485,024 between 2014 and 2015. This followed a year on year rise since 2010.
Colistin is also routinely given to treat cystic fibrosis patients who suffer repeat infections from resistant pseudomonas bacteria and other infections.
A "matter of life and death"
Rising colistin resistance was a “matter of life and death” for such patients, warned a spokesperson for the Cystic Fibrosis Trust. “Resistance means we’d lose one of our most effective antibiotics for prevention and treatment of infection in cystic fibrosis patients,” added Stuart Elborn, Professor of Respiratory Medicine at Imperial College.
One of the UK’s leading microbiologists told the Bureau doctors were prescribing more colistin because of rising superbug infections.
“The colistin use in itself is not concerning, but what is concerning is the rise in (...) infections and resistance,” said Professor Peter Wilson, consultant microbiologist at University College Hospital London.
“When you’ve got an infection you know is resistant to carbapenems you use colistin. It’s not an antibiotic doctors would use out of choice.”
Rise in dangerous superbugs
One type of CRE bacteria known as CPE, can live in the gut without making someone ill, but produces an enzyme which can break down whole classes of antibiotics, rendering them useless. After the government asked hospitals to look out for this particular bug in 2014, the number of bacteria samples sent to Public Health England rose by 15%. Cases of another type of bug which releases an enzyme which protects it from two main classes of antibiotics are also rapidly rising.
Rises in these types of infections inevitably means more colistin will be prescribed, microbiologists told the Bureau. The rise in colistin prescriptions can also be explained by doctors using higher doses of the drug - because once a bug has developed a level of resistance, more of the drug is needed to effectively kill it, according to Philip Howard, consultant pharmacist at Leeds Teaching Hospitals NHS Trust and spokesperson for the Royal Pharmaceutical Society.
Officially the rules on dosing for intravenous colistin changed this year. Doctors will have been prescribing higher amounts for years before this as these studies will have been circulated at conferences and training events, Mr Howard said.
He echoed concerns over increasing prescriptions leading to resistance. “The bottom line is the more you expose a bug to antibiotics it will try its damndest to become resistant to survive it. The more you use any antibiotic you risk resistance,” he told the Bureau.

Discovery of MCR-1
In late 2015 the discovery of a gene which makes bacteria resistant to colistin – called MCR-1 – sparked worldwide alarm. The gene was first discovered in pigs, human patients and retail pigs in China; other countries then went on to search their collections of stored bacteria and found MCR-1 was already present in countries all over Europe including the UK, the US, and in certain parts of Asia and Africa.
Colistin is widely used in farming, mainly as a growth-promoter (although using it in this way has been banned in Europe), making animals gain muscle faster while protecting them against disease at the same time. Despite its importance in human medicine, it is expected 16,500 tonnes of the drug will be sold worldwide by 2021. Scientists believe this rampant use in agriculture is why the MCR-1 gene developed and spread around the globe, breeding untreatable superbugs.
The discovery of MCR-1 prompted China - the greatest user of antibiotics in farming - to ban colistin as an animal feed additive and the European Union to recommend its usage in agriculture be slashed by two thirds. However the Bureau has discovered that the UK’s Veterinary Medicines Directorate, the body which regulates drugs for animal use, last year licensed three new products for use on British farms.
Licensing new products containing colistin for use on British farms was “sheer, utter madness,” said Professor Timothy Walsh, one of the scientists who originally discovered colistin resistance.
Colistin is likely to become useless as a drug within 10 years if its usage in veterinary medicine is not stopped, he warned. “The only way we can safeguard [colistin’s] use in human medicine is to ban it in husbandry and agriculture,” he told the Bureau.
Continuing to use colistin so widely in human medicine would also inevitably spur the growth of MCR-1, said Dr Weinbren, but doctors currently have no choice. There are few alternatives for treating CRE infections. A 30-year gap in antibiotic development means no new drugs will be brought to market in the next decade.
“The one thing you can be sure of is that the organisms will develop resistance,” he said. “It’s Darwinian. It’s as sure as eggs are eggs. Colistin resistance will become more common. When you’re down to one class of antibiotic, you’ve got to be worried. You’ve got to be terrified and we need to be doing something about this."
Fears of a 'post-antibiotic era'
Antibiotic resistance is already believed to kill hundreds of thousands of people around the world each year. The true figure is not known because of difficulties and failures in recording data.
Resistant infections already kill about 57,000 and 26,000 newborn babies per year in India and Pakistan respectively, according to academic studies. In the UK, at least 12,000 people die from antibiotic-resistant bugs each year, medical experts estimate - more than die of breast cancer.
Resistance has been fuelled by the overuse and misuse of antibiotics in human medicine and in agriculture, particularly factory farming. A concurrent failure by the pharmaceutical industry to create new antibiotics has compounded the crisis.
Last September saw leaders from around the world meet for an high-level United Nations summit on antibiotic resistance, also known as antimicrobial resistance (AMR). A five-point action plan was agreed, including improving the way antibiotics are used around the world and reducing infections.
The UK has been a key leader in the global fight against AMR and had already set its own targets in May 2016, including halving the amount of inappropriate antibiotic prescriptions in humans by 2020.
The total amount of antibiotics prescribed in hospitals in England did fall by 4% in 2015 - the first time this had happened. Prescribing in the community - where the bulk of antibiotics are given out - fell by 6%. This includes those given out by GPs, dentists, nurses, pharmacists and those written in hospital but dispensed in a pharmacy.
Experts have warned if nothing is done to protect the drugs that still work we may face a “post-antibiotic era” within decades. A scratch on the skin could become deadly and procedures like hip replacements, Caesarean sections and chemotherapy could become too dangerous because of the likelihood of infection.
The UK government also aims to reduce antibiotic use in livestock and fish farming by about 20% by 2018.
When it announced its AMR goals the Department of Health said it would “introduce strict oversight of the use in animals of antibiotics which are critical for human health – including supporting restrictions or even bans where necessary.”
In that context, Coilin Nunan of advocacy group Alliance to Save our Antibiotics said the VMD’s decision to license more colistin products to the animal market last year was "astonishing" and highly irresponsible.
A Government spokesperson said: 'UK doctors are making great strides in cutting antibiotic prescriptions. In animals, there are tight restrictions on the use of colistin and it is only used as a last line treatment where no other alternative exists. Defra continues to promote good hygiene and animal care to prevent the need for antibiotics to be used in livestock.'