
Drug company reps give quack doctors fridges and televisions to sell antibiotics
Two of India’s biggest drug companies are alleged to be giving inducements to “quack” doctors of gifts and cash to encourage them to prescribe vast amounts of antibiotics, fuelling the rise of drug-resistant superbugs around the world.
Undercover reporting by the Bureau has revealed that Abbott and Sun Pharma — whose products and devices are sold and used in more than a hundred countries, including in the US and by the NHS in the UK — promote antibiotics to healthcare practitioners who often have no formal medical training. It is illegal to sell antibiotics to quack doctors in most parts of India, but the law is rarely enforced. There are no restrictions on promoting the drugs to them.
These so-called quacks, who can be the only healthcare provider in their impoverished communities, often go on to prescribe antibiotics incorrectly. By offering incomplete or simply unnecessary treatments, they unwittingly speed up the creation of superbugs that kill tens of thousands of babies in India alone each year. An Abbott salesman suggested he knew the drugs might be misused, but he was motivated purely by profit.
A Sun Pharma salesman told an undercover Bureau reporter that quacks and real doctors were given high value gifts to encourage them not to switch to a competitor. These ranged from gift cards, medical equipment and fridges to televisions, travel and cash. Sales representatives would also offer extra pills or money as an incentive to buy more antibiotics, encouraging potentially dangerous overprescription.
Sun Pharma is the largest drug manufacturer in India, with more than £3bn revenue in 2018, and its products are used by the NHS. NHS rules do not prevent it buying from companies that give inducements to doctors, as long as none are given in the British supply chain. The NHS also buys devices from Abbott Laboratories, a US company that pulled in more than £24bn in revenue last year. Its Indian subsidiary, Abbott India, is the second-biggest pharmaceutical business in the country.
At Abbott, a salesman said that doctors and quacks were lured in with gifts worth up to 2,000 rupees (£23). The company also offered buy-five-get-one-free deals on boxes of antibiotics, encouraging bulk buying and consequently more prescriptions — “whether necessary or unnecessary,” he said.
India’s unqualified doctors — who are often from poor rural areas and slums — earn so little that these incentives can raise their monthly income by as much as a quarter. Abbott also offers doctors a taste of luxury, throwing surprise parties for their families and cocktail soirees in five-star hotels.
Spokespeople for both companies said that their policies prohibited offering gifts to healthcare providers to encourage prescriptions.
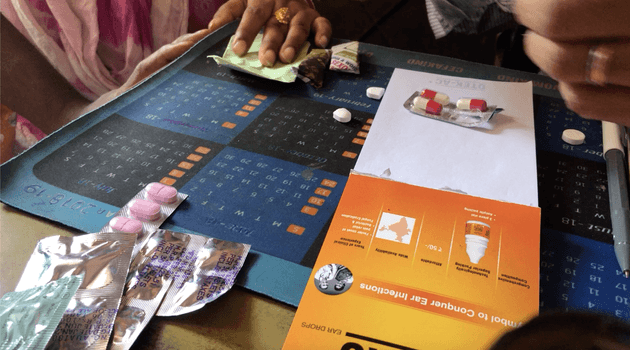 A quack doctor prescribes a combination of antibiotics and Ayurvedic medicines for a patient
A quack doctor prescribes a combination of antibiotics and Ayurvedic medicines for a patient
Rising use of antibiotics is the main cause of antimicrobial resistance (AMR), one of the world’s greatest health threats. Bacteria evolve resistance to drugs naturally over time, becoming superbugs, but mass or inappropriate use dramatically speeds up this process.
Experts condemned the pharmaceutical companies for encouraging incorrect use of antibiotics and selling to quacks, who contribute to AMR when they wrongly prescribe the drugs.
Lord Jim O’Neill, who led a global review of AMR, called the Bureau’s findings astonishing. He said: “Many pharmaceutical companies like to position themselves as being responsible and here is some rather frank evidence to the contrary.”
Professor Ramanan Laxminarayan, director of the Centre for Disease Dynamics, Economics and Policy (CDDEP), said: “When you consider that there are five times the number of rural medical practitioners in India as there are trained medical doctors, it should come as no surprise that the majority of antibiotics reach patients through this channel. It is no surprise that pharma companies push antibiotics through [them].
“There is a need to balance access to antibiotics, which these practitioners provide, and also prevent overuse and inappropriate use and therein lies the challenge.”
The Bureau newsletter
Subscribe to the Bureau newsletter, and hear when our next story breaks.

A crisis built on good intentions
India is the epicentre of the antibiotics resistance crisis. Superbugs kill at least 58,000 babies every year and Indian doctors warn they regularly see patients with “pan-resistant” infections; those resistant to all available drugs.
Simultaneously the country is struggling with a lack of access to basic healthcare, including antibiotics. In theory India offers free healthcare to its poorest citizens, but a recent report from the CDDEP found a shortfall of 600,000 government doctors and two million nurses.
Many people therefore depend on India’s more than 2.5 million quack doctors, which includes those who practise traditional medicine, such as Ayurveda, homeopathy and naturopathy, and those with no medical training at all. They vastly outnumber the one million private or government doctors trained in scientific medicine.
Often known as “uncles” or “chotto doctors”, which means small doctor, the quacks are deeply respected in their communities and consulted on everything from health problems to who their child should marry. Many patients do not realise the doctor they visit has no recognised qualifications.
The quacks provide some form of medical coverage in poor and rural areas that would otherwise completely lack healthcare. Every year more than half a million Indians die from treatable infections because they have no access to healthcare or life-saving drugs.
Sales representatives from Sun Pharma and Abbott who spoke to an undercover Bureau reporter made no secret of the incentives they offered quacks and doctors alike.
Abbott has been widely criticised in the past for expensive gifts to doctors, so the company has introduced restrictions — but staff found indirect routes around the rules. The salesman said workers had been told “we shouldn’t do it directly”, but that gifts and free samples were still commonplace in other departments. “In certain specialties they are going all out to offer whatever is possible,” he said.
Direct gifts to doctors and quacks are limited to 2,000 rupees (£23), but more expensive perks are given indirectly through training programs and third parties. Some doctors are paid up to 20,000 rupees (£230) to speak at conferences.
"Now, the point is not about whether they work or not. The point is: where is the market?"
The company even gives away free drugs, as samples or in deals. For every five boxes of antibiotics bought the company provides an extra box free. The sales representative said providing extra tablets usually led to more prescriptions, “whether necessary or unnecessary”.
He admitted that sales representatives promoted antibiotics based on how much profit they would make, rather than medical evidence. He said: “Now, the point is not about whether they work or not. The point is: where is the market? Where is the big market? [...] So it is not about the efficacy part, it is about how good I can grab the particular market and then penetrate into that market.”
At Sun Pharma, sales representatives are asked to visit up to a dozen “doctors” — real or quacks — every day. Half of their 200 regular customers are quacks, who experts say are frequently targeted more aggressively than conventional doctors.
The salesman described quacks as an “easy” market for antibiotics and their main target for sales. Professional doctors needed to be convinced of how safe and effective a drug is, whereas quacks often required no explanations, only incentives, he said.
“You can give any damn thing,” he said. “From a needle to a missile you can give any damn thing. They will accept it. And higher value is the input, higher value will be the output [...] It can be a TV. It can be a fridge. It can be any damn thing.”
The aggressive marketing is in part down to their sales targets: Sun Pharma sales representatives earn bonuses if they sell more than 300,000 rupees (about £3,440) worth of antibiotics and painkillers every month.
A spokeswoman for Abbott said it prohibits sales teams giving anything of value to doctors or pharmacists as incentives to sell its medicines and that the teams receive regular ethics and compliance training. She said sales staff “only meet with licensed health practitioners who are authorized to prescribe medicines”.
Sun Pharma said it was “surprised and saddened to hear about the views shared by an alleged Sun Pharma sales representative”. The company’s spokesman added: “We can categorically say that this person’s views in no way reflect Sun Pharma’s values and the alleged activities are contrary to our company policies. At Sun Pharma, there is no room for unethical conduct or non-compliance with applicable laws, rules and regulations.”
The company said that it did not allow gifts to healthcare workers that were “intended to have an inappropriate influence on [their] decision to prescribe, recommend, purchase, supply or administer products”. It added that staff breaking this rule, or any law, would face disciplinary action or dismissal.
Last year the Access to Medicines Foundation, a non-profit organisation seeking to widen access to healthcare in the global south, created the AMR Benchmark, a voluntary index rating 18 companies’ performance on measures agreed to reduce drug resistance.
It challenged companies to increase access to antibiotics for those who need them while taking measures to ensure they are used appropriately, mitigating the threat of resistance. Three companies — Glaxo, Shinogi and Pfizer — decided to bring in policies that clearly separated bonuses for sales staff from the amount of antibiotics they sell.
Dr Meenakshi Gautham, a researcher from the London School of Hygiene and Tropical Medicine based in India, has interviewed quacks, also called informal providers, for more than a decade and concludes they are being increasingly targeted by pharmaceutical companies who aggressively market antibiotics.
Make change possible
Investigative journalism is vital for democracy. Help us to expose injustice and spark change
Click here to support us“I have had pharmaceutical representatives tell me in some areas that if they have targets to sell 100,000 rupees [£1,150] worth of antibiotics, 80,000 comes from selling to informal providers, and 20,000 from formal doctors,” she said.
Her research shows that most quacks, as well as private doctors, get all their information about antibiotics from sales representatives and drug companies, rather than independent sources. Companies will host fully catered conferences for quacks with paid lectures from private doctors on which antibiotics to prescribe, she said.
She confirmed the practice of offering quacks free samples of antibiotics. They will often then give these to their poorest patients for free, as a misguided act of charity. The sample packets usually don’t contain a full course of antibiotics, making them less effective and ensuring patients don’t complete the treatment, which is known to fuel drug resistance.
“There is a strong push coming from the pharmaceutical industry,” Gautham said. “That push takes the form of very aggressive promotion of antibiotics, especially in rural markets, because these represent huge turnovers for those companies that manufacture and market antibiotics.
“Unless we work with the pharmaceutical industry to reduce the aggressive strategies, it’s going to be difficult to work only with the providers [quacks] and get them to reduce their use.”

Inside a quack doctor's clinic
Down a narrow road in Ambedkar Nagar, a poor area of Delhi, patients wait to see Doctor Chullan*. There is a pile of rubble opposite his clinic, and from inside you can hear car horns, motorbikes and the shouts of men pushing carts of fly-covered fruit.
Chullan is examining Jayati*, 22, a young woman in a yellow sari who has come to the surgery with her two young daughters. “I stood in the rain and took a bath and now I have a cold and fever,” she says as he takes her temperature.
He prescribes her four antibiotic tablets, a paracetamol, and some yellow and green Ayurvedic pills. Ayurveda is a traditional system of healing practised in India and Chullan has jars of its medicines, including brightly coloured tablets, powders and dried leaves, on his shelves. Boxes of drugs — antibiotics, vitamins and painkillers — are stacked on another bench, some grey with dust.
Chullan has a degree in Ayurveda but no recognised qualification in scientific medicine, which means he is prescribing antibiotics illegally.
Later, Chullan tells another woman to buy three antibiotic tablets from the pharmacy for toothache, although there is no evidence she has an infection or abscess, and a proper course of the drug should last seven to ten days.
A few miles away, hospitals face crippling rates of antibiotic resistance.
*Names have been changed to protect anonymity
Header image: Sun Pharma's headquarters in Mumbai, by Amit Madheshiya/Bloomberg via Getty Images
Our reporting on anti-microbial resistance is part of our Global Health project, which has a number of funders. Our work on superbugs (to December 2018) was funded by the European Journalism Centre. None of our funders have any influence over the Bureau’s editorial decisions or output.




