
Revealed: Thousands more deaths in home care during pandemic
More than 25,000 people in England who received care in their own homes died, with reported deaths doubling in many areas
Four times a day, every day, Nicky is visited at home in London by her care workers. She is 54 and has multiple sclerosis, learning difficulties and schizophrenia, a complex set of needs that means two care workers see her for each visit. Without them, she would not be able to get out of bed. “She's pretty much entirely dependent on them. Nicky’s carers are fundamental to her having a normal life,” a relative said.
When lockdown was first imposed, Nicky’s family noticed the lack of PPE care workers were using around her. A relative recalls care workers not wearing gloves, and telling him they were buying their own masks because those provided by their agency cut into their ears painfully.
In other moments, the crisis encapsulated where Nicky’s care had already been poor and spotty. Her relative said: “There’s no clear doctrine or approach to hygiene with Nicky anyway, or dealing with injuries, or to people with mental illness, or learning disabilities … That’s the strange, yet very familiar feeling I have, because the same kind of inconsistent and fairly lax approach to her is also their approach to a global pandemic, and their [staff’s] working conditions.”
Home care, or domiciliary care, is vital for hundreds of thousands of people across the UK. But despite home care serving some of the most vulnerable people in the country, the pandemic’s impact on the service, and on its clients’ health, has received a fraction of the attention paid to residential care homes.
The first official statistics covering the deaths of those receiving home care over the past year suggest that the pandemic has taken a great toll on a stretched and unequal system. More than 25,000 people died in the past year while receiving home care in England, and almost 3,000 died over that period in Scotland, the Bureau of Investigative Journalism can reveal.
These figures suggest reported deaths increased in England by nearly 50% between April last year to March, compared with the previous year. The deaths will include elderly people, those with physical and learning disabilities, and mental health conditions — all people who rely on care workers coming into their own homes for them to be able to live independently. This rise in reported deaths in England of 50%, and in Scotland of 70%, compares to an increase of 22% in the wider population in England, according to figures from the ONS.
Although recorded deaths have climbed, relatively few people in home care have died of coronavirus. Across England, the data suggests only 8.7% were Covid-19 related, though that rose to 20% in some areas.
The data shows very wide regional differences in deaths across England. In this, it appears to reflect the fragmented, complex home care system, where care can be delivered through one of almost 19,000 providers, including agencies, non-profits, councils, NHS trusts and clinical commissioning groups.
Deaths of adults in home care more than doubled in 38 council areas across England, according to data from the Care Quality Commission (CQC). In ten local authority areas recorded deaths tripled.
One of those areas is Liverpool, where 358 deaths were recorded over the past year of the pandemic, up from 100 in 2019. A Liverpool council spokesperson told the Bureau that despite the figures, Covid-19 cases among those in home care had remained low during the pandemic, only picking up in the last wave, and confidence in domiciliary care remained high. They suggested more people now need care at home and fewer are in residential care.
Fazilet Hadi, of the charity Disability Rights UK, told the Bureau: “The dramatic increase in deaths of people receiving domiciliary care during the pandemic appears to be truly shocking. It is very important that the figures are further analysed.
“Disabled and older people receiving care at home can often be very isolated and forgotten by the world around them. The everyday challenges they face are largely invisible and it is time we put a spotlight on their experiences during the pandemic.”
Unnumbered, invisible
Bureau Local gathered its data via Freedom of Information requests from the CQC, England’s care regulator, and its equivalent in Scotland, the Care Inspectorate, and compared this to 2019 data published by the ONS. Breaking down the data by local authority revealed the vast differences in trends across England.
Not all those being supported at home who die are captured in the figures. By law, deaths have to be reported to the CQC by a care provider if a person died as a result of their care or if a care worker was in their home at the time. But that fails to take account of those who die when only family are present, or the millions of people who are solely cared for by unpaid family members and friends.
Care providers can still choose to report other deaths to the CQC but there is no obligation, and the CQC told the Bureau it was aware that reporting varied greatly between providers, regions and over time. The United Kingdom Homecare Association, which represents home care providers, suggested one of the reasons for the steep rise in reported deaths could be that providers were reporting more deaths to the CQC "on a precautionary basis" during the pandemic, even when they were not strictly required to.
It is difficult even to find comprehensive data on the number of people receiving home care, because of the mix of those whose care is paid for and organised by local authorities, and those who pay for their own personal assistants. Social care, unlike NHS healthcare for most people, is not free at the point of service, and is needs and means tested across most of the UK, with eligibility criteria varying across local authorities. Records from 2018 suggest at least 500,000 people were receiving some form of council-funded home care.
 Tracking the number of people who receive care at home is difficult, because many self-fund their own care, or are cared for informally by friends and relatives
Jason Alden/Bloomberg via Getty Images
Tracking the number of people who receive care at home is difficult, because many self-fund their own care, or are cared for informally by friends and relatives
Jason Alden/Bloomberg via Getty Images
While a major study is underway into the impact of Covid-19 on care homes, there is no equivalent focus on those receiving care at home. However, the Bureau’s reporting has found that a lack of PPE, slow vaccination take-up among some care workers, and Westminster’s failure to prioritise funding for home care may all have contributed to the sharp rise in deaths in some areas.
Hadi said: “We know that the use of PPE and testing was slow in reaching domiciliary care and that this is likely to have contributed to the deaths of older and disabled people receiving support at home and care workers.
“However, the figures appear to show that the majority of deaths weren’t due to Covid and it is important that we clarify whether causes of death were wrongly recorded or whether other factors were at play. We know that many people receiving social care experienced cuts to their care and the link between these reductions and the higher rate of deaths also needs exploring.”
The government’s “Protect the NHS” message may have caused people to avoid hospital treatment, and could have meant families kept relatives at home.
The United Kingdom Homecare Association said: “Official data also show that whilst excess deaths at home were higher during the pandemic, those in hospices decreased ... We believe it likely that during the pandemic, more people chose to die at home, in familiar surroundings with the right care and support, than in hospices or hospitals than in previous years.
“The work undertaken by TBIJ highlights the lack of publicly available, complete and consistent data sets related to homecare, as in so many other areas of social care, which would help illustrate trends. High quality data enables policymakers to make decisions about areas where actions would benefit citizens. We believe that it would be extremely helpful for the government to consider the data it collects in relation to social care.”
A disease of inequality
The Bureau has spoken to dozens of care organisations, charities, local authorities and families about their experiences of home care during the pandemic.
Shelagh Thompson lives in Birkenhead with her husband and two sons, David, 26, and Karl, 25, who are both severely disabled. Until March last year, she had been generally happy with her sons’ care.
 Shelagh Thompson with her husband Pete and her sons Karl and David, who both require support from care workers
Victoria Tetley for TBIJ
Shelagh Thompson with her husband Pete and her sons Karl and David, who both require support from care workers
Victoria Tetley for TBIJ
“Before Covid,” she said, “Wirral council had been giving me enough hours. At the time there were four full-time care workers between the two of them, four full-time care workers and two part timers, and of course, there was also me. I'm part of the team too, but no informal carer gets paid. We do the same work, but we don't get paid.”
But then Thompson and her family experienced a huge reduction in care last year when, due to the pandemic, one of their care workers left the industry, and another went home to care for their own family. David was unable to wear a mask, which restricted how much care he could receive. “It was devastating really,” Thompson told the Bureau.
One of the care workers agreed to move in with the family, and other support workers helped by dropping off shopping and playing chess online with Karl. But life was much more difficult inside a packed house with no respite care and less support. “We just had to do what everyone else had to do — dig in and get on with it … It was terrifying to be honest because if I got Covid, I thought: ‘What on earth is going to happen?’”
 David with Josh, a care worker who moved in with the Thompsons during the pandemic to support them
Victoria Tetley for TBIJ
David with Josh, a care worker who moved in with the Thompsons during the pandemic to support them
Victoria Tetley for TBIJ
 Josh was given an award for his dedication to the family
Victoria Tetley for TBIJ
Josh was given an award for his dedication to the family
Victoria Tetley for TBIJ
In Bury, the number of recorded deaths of home care recipients more than doubled year-on-year during the pandemic, and it is one of the areas with the highest rise in deaths according to the CQC figures. However, the council’s own data, obtained under FOI, shows the council recorded a much higher number of deaths in this group than were reported to the CQC: 179, of which 24 deaths involved Covid-19. (Councils generally receive notice of more deaths than the CQC due to differences in data collection.)
A spokesperson from Bury council said the figures reflected “people’s choice in where to spend their latter days”, adding that people who might usually have sought hospital treatment or moved into a care home or hospice may have been restricted from doing so, or been put off by care homes forbidding visitors during lockdown.
The unequal picture across different areas raises questions about how local circumstances have affected home care. Relative levels of deprivation, pre-existing health inequalities, and existing strains on adult social services are important factors to consider. A 2020 survey of nearly 150 council directors of adult social services revealed just 4% of them were confident their budgets were adequate enough to meet their legal duties.
Anna Hartley, director of public health for Wakefield council, described Covid-19 as a “disease of inequality that has been pretty devastating for areas like Wakefield”.
She said: “When we look at our domiciliary care cases, they’re also disproportionately from those deprived communities. In Wakefield, 89% of our domiciliary care users are fully funded by the local authority. Because a person has to be on a fairly low income to become fully funded, this means our domiciliary care users tend to be more deprived or on a fairly low income. Also, if you look at age, which is the main risk factor for Covid, only 16% of our cohort are under 64.”
She added: “It feels to me like quite an unbalanced system because social care does need more energy and support at a national level, and I think at a local level, where people are passionate about it, they want to see that.”
Join the Bureau Local
Become part of the Bureau Local — our collaborative network of reporters and citizens — and tell stories that matter
Find out moreAs the UK at large follows the government’s roadmap out of lockdown, improvements in home care may be slow to follow. The CQC figures obtained by the Bureau show a trend of sustained higher levels of reported deaths well into 2021 and the second wave of the pandemic, in spite of the fast vaccine rollout.
Moreover, government data shows that in some areas of England, vaccination rates of CQC-registered home care workers were as low as 39% (as of 29 April). The rate was lowest in Hackney, London, but 11 other local authorities had fewer than half of their workers vaccinated with at least one dose by the end of April.
Crisis after crisis
Public satisfaction with care services in Britain is very low, even as demand looks set to rise as the population ages. The London School of Economics predicts that about 29% more adults between 18 and 64, and 57% more aged over 65, will need care in 2038 compared with 2018.
Even before the pandemic, the sector was in a state of financial crisis. Not accounting for the impact of Covid-19, the social care funding gap is estimated to be anywhere between £1.4bn and £12.2bn per year.
Since the pandemic made these shortcomings clear, the issue has been climbing the political agenda, with Labour calling for urgent legislation to be included in tomorrow’s Queen’s Speech. Boris Johnson said last week that social care in England was “a massive priority” and that plans for the long-term funding of the sector would be brought forward. In Scotland, there are proposals for a National Care Service, and ending charges for personal care at home.
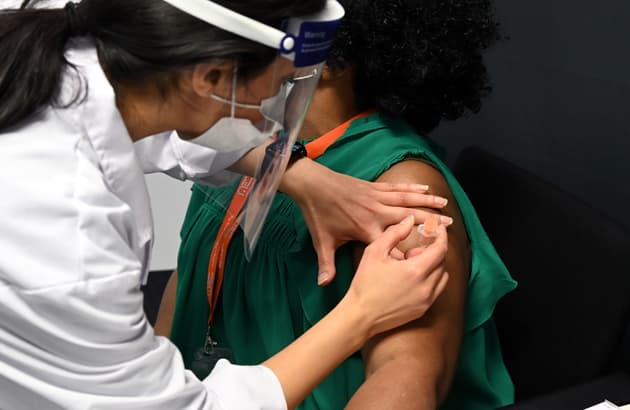 A care worker is vaccinated in Borehamwood. In some areas, fewer than half of home care workers have had their first jab
Karwai Tang/Getty Images
A care worker is vaccinated in Borehamwood. In some areas, fewer than half of home care workers have had their first jab
Karwai Tang/Getty Images
Eleanor Lisney, the co-founder of disability collective Sisters of Frida, describes the UK social care system as a postcode lottery. “Each local authority decides differently. Even next door boroughs can have a different assessment and payment system.”
Lisney needs assistance at her home in Greenwich, London, to help with cooking and domestic tasks; for example, it is not safe for her to handle a hot kettle.
During the pandemic, her arrangements were disrupted: “I had to change one [assistant] because of his own study needs, which required him to use public transport, and furlough another because she had her own family duties.” In an ideal world, she said, care would mean that “we would have the assistance we need — good, intelligent assistance which is regular”.
Care workers, and their representatives, point to systemic problems with funding and pay that damage the quality of care they can provide. Gavin Edwards, Unison’s senior national officer for social care, told the Bureau: “Until the government overhauls the sector and provides the funding it desperately needs, unscrupulous employers will continue to put lives at risk.
“Many domiciliary carers are paid the minimum wage and hold unstable zero-hours contracts. Throughout the pandemic, staff have been going into people’s homes with nowhere near enough PPE, while guidance they’re given shows no understanding of their roles. What’s more, testing has been woefully inadequate.
“Many have been under significant pressure to carry on when they should have been isolating because employers didn’t offer proper sick pay.”
Michele Vaughan, who left care work in March of this year, agrees. She told the Bureau: “I know of one girl who was absolutely ripped apart because her husband was self-isolating. He only got statutory sick pay, and she said: ‘If I don’t come to work, I cannot put food on the table next week.’ ”
At one home, she discovered an elderly client had a catheter whose urine leg bag had not been changed by care workers in more than a week. Vaughan said a culture of poor pay, staff shortages, and overall declining standards had contributed to the horrifying things she has witnessed, which eventually prompted her to leave the job. She told the Bureau she feared the concerns she had would only be addressed after clients died. “That's the sad situation. It’s inevitable. Sooner or later, somebody will die.”
Do you have experience of the home care system? As we continue to explore this area we want to connect with people directly affected - from those receiving assistance, those who work in home care, those caring for relatives and/or involved in advocacy.
Reporting team: Vicky Gayle, Rachel Hamada, Charles Boutaud
Community organising team: Eve Livingston and Emiliano Mellino
Bureau Local editor: Emily Wilson
Investigation editor: Meirion Jones
Production editor: Frankie Goodway
Fact checker: Gareth Davies
Data checker: Ben Stockton
Our reporting on health inequality is part of our Bureau Local project, which has many funders. None of our funders have any influence over the Bureau’s editorial decisions or output.
Header image: An elderly woman at the pensioners' parliament event in 2006. Credit: Christopher Furlong/Getty Images
-
Area:
-
Subject:




