
Health inequality – what next?
The second year of the pandemic once again exposed health inequalities across the UK, as the public realised where they lived and how they worked hugely influenced their levels of risk. More than ever, access to the right health information – whether about variants or vaccinations – was critical.
It was to explore these very issues that Bureau Local’s Health Inequality beat was launched a year ago. Health injustice has increased in the UK over the past decade, leading to wildly different outcomes for different people and communities – as laid out in national reports, such as the Marmot Review 10 Years On.
But what has become increasingly clear throughout our year of reporting is that most health inequality in the UK is created by events and circumstances long before people reach the doors of a GP’s surgery or hospital. We now want to take what we’ve learned over the past year and examine wider social inequality, while always keeping in mind the potential health outcomes for those left disadvantaged by systemic injustices.
We are very grateful to those of you who collaborated with us and helped shape the following investigations:
Deaths in home care
Our first investigation was into the deaths of people who receive care at home during the first lockdown. While there had been some excellent reporting on deaths in care homes, with inquiries launched, little had been done on people who receive care in their own homes – nor was there much publicly available data.
We used Freedom of Information requests to gather data on these deaths and revealed that people had been dying at a much higher rate than expected, with most of those deaths not linked to Covid-19. Reported deaths of adults in home care more than doubled in 38 council areas across England, according to data from the Care Quality Commission, and in 10 local authority areas the number of deaths tripled.
We published our findings alongside Disability News Service and the story also appeared in i news, The Times’ print edition and The Ferret, as well as local publications from Liverpool to Haringey in London. We also worked collaboratively with Contemporary Narratives Lab and theatremakes Coney on HOME/CARE, a creative experience based on the testimonies of people receiving home care during the pandemic.
Disability Rights UK’s Fazilet Hadi told the Bureau: “The dramatic increase in deaths of people receiving domiciliary care during the pandemic appears to be truly shocking. It is very important that the figures are further analysed.
“We know that many people receiving social care experienced cuts to their care and the link between these reductions and the higher rate of deaths also needs exploring.”
The vaccine maze
Once the vaccination programme launched, our sources told us people were struggling to get jabbed without being registered with a GP. They added that surgeries were often refusing to register undocumented migrants – against NHS policy.
To gather evidence we called practices in 10 key cities around the UK to find out if they would register an undocumented patient. Most of them would not, and access to drop-in centres had been confusing and fragmented, meaning that undocumented people in the UK often had few options when it came to protecting themselves and their families from Covid-19.
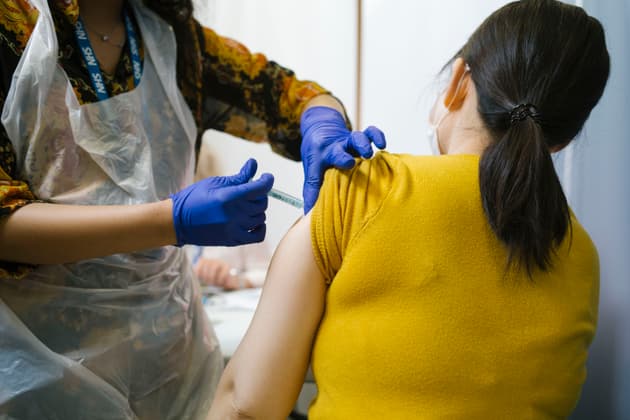 A vaccination pop-up clinic
Alex Sturrock for TBIJ
A vaccination pop-up clinic
Alex Sturrock for TBIJ
We worked with The Independent and Channel 4 News to tell this story. Our findings were also covered by African Voice, South China Morning Post, on Express News TV for the Latin American community in the UK, and on BBC World Service. TBIJ’s Global Health team also investigated the issue of vaccine access for undocumented migrants across Europe. Our community organiser, Emiliano Mellino, and Bureau fellow, Sarah Haque, both wrote in more detail about the investigation: Emiliano on how we can work with grassroots groups to investigate health exclusion and Sarah on From Glasgow to Galicia: How Vaccine Rollouts are Leaving Migrants Behind.
By helping to strengthen the advocacy of organisations like Doctors of the World, we saw impact. For example, many people wrote to their MPs to demand change and many more GP surgeries signed up to the Safe Surgeries initiative. Our findings were cited in Parliament by Virendra Sharma MP while the NHS Race and Health Observatory called for an “urgent investigation” to address the problem.
When is a House Not a Home?
For our final health inequality investigation, we have come full circle to where we began: people’s homes. We are busy data crunching and speaking to disabled residents whose homes are not fit for their needs and desperately need adapting.
One of the main messages to have emerged from our health inequality work over the last year is the extent to which disabled people are systematically prevented from living life as fully as they should be able to. This is something we want to take into our ongoing work and continue to scrutinise. So too is the fact that many health inequalities are intersectional and cannot be analysed in isolation.
What now? Inequality across all our investigations
Many complex, interconnected factors such as economic inequality, job insecurity, unequal treatment in the justice system, variance in quality of education, poor housing, local decision-making, racism and discrimination ultimately lead to people experiencing worse health in their lifetimes and dying younger. More than a decade of austerity and cuts to services have also taken their toll.
So rather than reporting on health services at the point of delivery, which is important in itself, meaningful journalism on health inequality needs to get to the heart of why some groups of people experience much worse health outcomes than others and what it means to live this reality on a daily basis.
For that reason, we have decided to refocus our attention. Rather than having health inequality as a separate beat, we are going to bring it into our wider work by investigating social and economic inequality in the UK and the people under most pressure as a result.
As the government starts to present its new focus on “levelling up”, we aim to examine the ongoing barriers to achieving equal economic and social conditions. By looking at stories where issues such as housing, health, care, employment, justice and local government meet, and by reporting with the people affected, we think we can shine a light on the realities of living in a post-Brexit, Covid-impacted UK.
So here are the projects we will be working on with our Bureau Local colleagues that encompass our mission for 2022. Feel free to tell us what you think we should be investigating on these topics:
Levelling Up – What do the projects being given extra funding actually mean for reducing inequalities? What are the untold stories of geographical differences in the access and provision of services and infrastructure? What should we dig into that would help communities to “level up”?
Justice For All – Our work on possession courts exposed the complexities of an under-reported area of the law. Who else is facing barriers to justice and how is it affecting their lives?
Is Work Working? – Who are the workers facing hidden disadvantages? How is the world of work changing and to the benefit of whom? We exposed systemic low pay at Deliveroo and the broken promises on zero-hours contracts at Amazon. What is next?
For those of you who have been with us from the beginning – we appreciate and thank you. For the people who have engaged with our work through our stories and our Health Inequality Lab events, we have hugely enjoyed working with you. We hope you stay in touch with us through the Bureau Local newsletter and continue to tell us what matters to you most where you live.
Reporters: Rachel Hamada and Vicky Gayle
Bureau Local Editor: Emily Wilson
Production Editor: Frankie Goodway
Photographs: Alex Sturrock
Header image: Two health workers consulting at a vaccine pop-up clinic
Our reporting on health inequality is part of our Bureau Local project, which has many funders. None of our funders have any influence over the Bureau’s editorial decisions or output.




